- Home
- About Journals
-
Information for Authors/ReviewersEditorial Policies
Publication Fee
Publication Cycle - Process Flowchart
Online Manuscript Submission and Tracking System
Publishing Ethics and Rectitude
Authorship
Author Benefits
Reviewer Guidelines
Guest Editor Guidelines
Peer Review Workflow
Quick Track Option
Copyediting Services
Bentham Open Membership
Bentham Open Advisory Board
Archiving Policies
Fabricating and Stating False Information
Post Publication Discussions and Corrections
Editorial Management
Advertise With Us
Funding Agencies
Rate List
Kudos
General FAQs
Special Fee Waivers and Discounts
- Contact
- Help
- About Us
- Search

The Open Clinical Cancer Journal
(Discontinued)
ISSN: 1874-1894 ― Volume 5, 2011
Significance of CEA and VEGF as Diagnostic Markers of Colorectal Cancer in Lebanese Patients
Hashem A. Dbouk1, 3, Ayman Tawil2, Fahd Nasr1, Loucine Kandakarjian2, Raghida Abou-Merhi*, 1
Abstract
Carcinoembryonic antigen and vascular endothelial growth factors are among the most important prognostic markers of colorectal cancer. Testing for these markers independently has been of limited value in screening for this tumor. The aim of this study is to determine the importance of simultaneous blood CEA and VEGF level determinations in diagnosis of colorectal cancer. Thirty-six patients diagnosed with colorectal cancer along with eight healthy controls were tested by ELISA for CEA and VEGF levels in serum and plasma, respectively. The positive predictive value of these markers was 95.4% for CEA and 89.5% for VEGF, and for combined CEA and VEGF was also high at 88%. Combined CEA and VEGF blood level assay constitutes a useful panel in detecting patients with colorectal cancer. Positive results allow selection of a subgroup of patients with a high tumor risk; therefore, such tests comprise valuable tumor diagnostic tests to add to current detection methods.
Article Information
Identifiers and Pagination:
Year: 2007Volume: 1
First Page: 1
Last Page: 5
Publisher Id: TOCCJ-1-1
DOI: 10.2174/1874189400701010001
Article History:
Received Date: 24/8/2007Revision Received Date: 27/8/2007
Acceptance Date: 22/10/2007
Electronic publication date: 8/11/2007
Collection year: 2007
open-access license: This is an open access article licensed under the terms of the Creative Commons Attribution Non-Commercial License (http: //creativecommons.org/licenses/by-nc/3.0/ which permits unrestricted, non-commercial use, distribution and reproduction in any medium, provided the work is properly cited.
* Address correspondence to this author at the Departments of Biology and Biochemistry, Faculty of Sciences I, Lebanese University, Hadath, Lebanon; Tel: +961-3-430515; Fax: +961-5-460796; E-mail: ra98@aub.edu.lb
| Open Peer Review Details | |||
|---|---|---|---|
| Manuscript submitted on 24-8-2007 |
Original Manuscript | Significance of CEA and VEGF as Diagnostic Markers of Colorectal Cancer in Lebanese Patients | |
INTRODUCTION
Colorectal cancer is the second most prevalent cancer and the fourth leading cause of death [1]. In Lebanon, it is the second most frequently diagnosed cancer in women and the fourth most frequent cancer in men; with a yearly incidence of about 12 cases per 100,000 individuals [2, 3]. The literature on colorectal cancer in Lebanon is limited and mostly related to its epidemiology. The tumor tends to be diagnosed in its late stages, which underscores the need for more effective detection methods [4-6].
Advances in molecular medicine, specifically in the areas of gene expression and proteomics have made it possible to correlate disease stages with molecular marker profiles. In the case of colorectal cancer, a wide variety of molecular markers have been studied. These studies have mainly focused on carcinoembryonic antigen (CEA), and more recently on vascular endothelial growth factor (VEGF), both of which are found in body fluids including serum and plasma [7-9].
Carcinoembryonic antigen (CEA) is a glycoprotein with a molecular weight of approximately 200 kDa [10, 11]. This antigen is expressed in a number of normal tissues including colon, stomach, tongue, esophagus, cervix, sweat glands, and the prostate [11]. In colorectal cancer however, its concentration is increased and the general distribution of the molecule on the cell surface is also altered. CEA is considered as one of the most clinically significant tumor markers for colorectal cancer, providing information on prognosis, tumor recurrence, and metastasis [10, 11].
Vascular endothelial growth factor (VEGF) is a dimeric glycoprotein of 34-42 kDa. It is expressed by a variety of normal cells, but is significantly over-expressed by malignant tumors (such as colorectal adenocarcinoma), where it can be produced by the tumor cells themselves or by stromal cells [12, 13]. This glycoprotein plays a crucial role in many pathologic conditions and malignancies because it stimulates capillary tube formation, endothelial cell proliferation, tumor invasion and metastasis, thereby playing an essential angiogenic role pivotal for tumor growth and aggressiveness [13-15].
The aim of this study is to measure the levels of CEA and VEGF in serum and plasma respectively in order to determine whether they can play a role in detection and diagnosis of colorectal cancer in the Lebanese population.
MATERIALS AND METHODOLOGY
Our study consisted of patients and controls, both of which are representatives of the Lebanese population with its cultural and religious diversity. The first group comprised of thirty-six patients with colorectal carcinoma (20 males and 16 females, mean age 67 years, age range 24 to 90 years) diagnosed at the American University of Beirut Medical Center (AUBMC) between October 2004 through June 2007. The control group consisted of eight healthy volunteers (6 males and 2 females, mean age 40 years; range 25 to 61) that were studied during the same period. Serum and plasma from the patients and controls were obtained and evaluated for CEA and VEGF levels.
At the time of enrollment in the study, 7 to 10 milliliters of whole blood were drawn from the anticubital vein from each patient preoperatively, and from each control individual after clinical evaluation. Blood samples were drawn separately into vacutainers containing sodium ethylenediamine tetra-acetic acid (EDTA-Na) for plasma and non EDTA-Na vials for serum. The samples were then centrifuged at 3500 rpm for 3 minutes (directly after extraction for plasma, and after waiting at room temperature for 20 to 30 minutes for serum), and then stored at -80° C until analyzed.
CEA serum concentration was determined by quantita-tive enzyme-linked immunosorbent assay (ELISA) (IBL CEA ELISA, Immuno-biological laboratories, Hamburg, Germany). VEGF plasma concentration was also determined by quantitative ELISA (Quantikine, R&D Systems, Minneapolis, USA). All samples were run in duplicate. The experiments were repeated three times and calculations were based on mean values in order to ensure accuracy.
Plasma samples instead of serum samples were used for VEGF levels in order to avoid inaccuracy resulting from the well known production of VEGF by platelets, thereby mak-ing the results more reliable and reproducible [16].
Statistical analysis was performed by Student’s t-test for independent samples using SPSS 15.0 for Windows statistical software, with α< 0.05 considered as statistically significant. Analysis included the following variables: CEA and VEGF levels, patient gender, age, tumor location, lymph node involvement, and presence of distant metastasis. Serum levels of CEA and plasma levels of VEGF were considered as pathological when they exceeded the mean plus two standard deviations of the control groups.
RESULTS
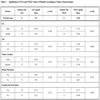
Patient characteristics are summarized in Table 1. CEA levels were assayed in all 36 patients, whereas VEGF levels were assayed in 27 of the 36 patients. The relatively small sample size is a reflection of the incidence rates of cancers in Lebanon, due to the small population size, as well as the low detection frequencies as many cancers go un-noticed or are diagnosed at terminal stages. Therefore, this provides direct evidence for the need to devise easy and cheap methods for cancer detection in the Lebanese population.
The cut-off values for both CEA and VEGF were calculated as the mean values obtained from the control cases plus 2 standard deviations. CEA levels < 3.8 ng/ml and VEGF levels < 12.84 ng/ml were considered normal.
The median CEA levels in patients and controls were 15.13 ng/ml (range 2.53 to 176.51 ng/ml) and 2.52 ng/ml (range 1.31 to 3.218 ng/ml), respectively. The median VEGF levels for patients and controls were 21.22 ng/ml (range 3.82 to 55.82 ng/ml) and 4.52 ng/ml (range 1.375 to 9.61 ng/ml) respectively (Fig. (1 ). Forty-eight percent of the patients had lymph node metastasis and 50% of the patients had distant metastasis. Both metastatic groups had CEA and VEGF levels that were higher than those of controls, but this difference was not statistically significant (p > 0.05). With respect to tumor differentiation, CEA and VEGF levels were near the cutoff levels in well-differentiated tumors, and much higher in moderately to poorly differentiated tumors, however, we were unable to include this in our study due to very limited number of patients with well-differentiated tumors (2 of 30) compared to moderate-poorly differentiated tumors (28 of 30), thereby preventing statistical comparison.
). Forty-eight percent of the patients had lymph node metastasis and 50% of the patients had distant metastasis. Both metastatic groups had CEA and VEGF levels that were higher than those of controls, but this difference was not statistically significant (p > 0.05). With respect to tumor differentiation, CEA and VEGF levels were near the cutoff levels in well-differentiated tumors, and much higher in moderately to poorly differentiated tumors, however, we were unable to include this in our study due to very limited number of patients with well-differentiated tumors (2 of 30) compared to moderate-poorly differentiated tumors (28 of 30), thereby preventing statistical comparison.
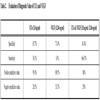
Using the cut-off levels mentioned above, specificity was 85.7% for CEA and 71.4% for VEGF, while sensitivity was 58.3% for CEA and 63% for VEGF. Independently, both markers had a high positive predictive value of 95.4% and 89.5% for CEA and VEGF respectively, and when combined, their positive predictive was also relatively high at 88%. The negative predictive value of these two markers was low, 28.5% for CEA and 33.3% for VEGF. The combination of both markers (using our cut-off values and those used in other studies) also gave a very low negative predictive value at 28% (Table 2).
DISCUSSION
Among the prognostic and diagnostic markers studied in colorectal cancer, the most significant are CEA and VEGF. They are linked to tumor growth and metastasis as well as other tumor properties [8, 11, 14]. VEGF plays a key role in angiogenesis, a highly complex process that is essential for tumor growth. Angiogenesis is regulated by various proand anti-angiogenic factors. One of the most important proangiogenic factors is VEGF, which is secreted by a variety of tumors and is regulated by the tumor cells themselves as well as by the tumor microenvironment [12, 14]. CEA, on the other hand, plays an important role in tumor metastasis, especially to the liver, where it mediates tumor cell adhesion to new sites [11].
Determining the relationship between these two and colorectal cancer, has been the focus of several studies. The results were variable in terms of their role in this tumor as either diagnostic or prognostic markers. Schiemann and coworkers showed higher levels of CEA in hereditary nonpolyposis colorectal cancer, and lower levels in sporadic colorectal cancer [18]. A review of various studies concludes that CEA has little diagnostic value; rather it has significant prognostic value in determining patient outcome following surgery or chemotherapy [10]. Still other studies show that the prognostic role of CEA in colorectal cancer may be enhanced with simultaneous use of other markers [18-20]. A recent study by Ferroni and coworkers showed that the use of tissue CEA and VEGF levels is potentially useful for the prognosis of colorectal cancer patients [21].
Studies have also produced conflicting results concerning VEGF as a diagnostic marker in colorectal cancer. Broll and coworkers demonstrated that VEGF has a low sensitivity of 36% [15], whereas our study shows a higher VEGF sensitivity (63%). Other studies showed that VEGF has a significant prognostic role by affecting the tumor’s metastatic potential, and by correlating with response to treatment and survival [16, 22, 23]. Preoperative and postoperative VEGF levels were also shown to correlate with prognosis [24]. Still other studies showed that the combination of CEA and VEGF increases the sensitivity in detecting colorectal cancer [15, 21, 25].
This study compares the significance of CEA and VEGF blood levels, both independently and in combination, as diagnostic markers for colorectal cancer. We found VEGF levels to be much higher in our patient group than in controls when compared to CEA. Most patient CEA levels, in contrast, clustered relatively close to the normal cut-off value of 3.8 ng/ml (or log[CEA] = 0.58) (Fig. (1 )). Furthermore, our findings differ from those of other studies, which demonstrate that the combination of both markers increases their positive predictive value. In our study, the use of individual markers gave a higher positive predictive value than the combination of the two markers at the selected cutoff limits. Lowering the CEA cut-off value to the 2.5 ng/ml figure used in a multitude of other studies as the cut-off value of preference for CEA, while maintaining our VEGF cut-off value of 12.84 ng/ml, increased the combined positive predictive value from that observed with our cutoffs (88%) to 89.5%. The low negative predictive values of these two markers in the Lebanese population indicates that results from such test should serve only as preliminary tests, and should be followed by others in case of suspicion of cancer or family history.
)). Furthermore, our findings differ from those of other studies, which demonstrate that the combination of both markers increases their positive predictive value. In our study, the use of individual markers gave a higher positive predictive value than the combination of the two markers at the selected cutoff limits. Lowering the CEA cut-off value to the 2.5 ng/ml figure used in a multitude of other studies as the cut-off value of preference for CEA, while maintaining our VEGF cut-off value of 12.84 ng/ml, increased the combined positive predictive value from that observed with our cutoffs (88%) to 89.5%. The low negative predictive values of these two markers in the Lebanese population indicates that results from such test should serve only as preliminary tests, and should be followed by others in case of suspicion of cancer or family history.
CONCLUSION
This study indicates that the combination of serum CEA and plasma VEGF levels, interpreted with the cut-off levels used here, appears to have value in the detection of colorectal cancer in our group of patients, and potentially for Lebanese and other patients. This is by no means a specific test since CEA itself may be detected in a variety of tumors such as lung and breast carcinoma, among others [11]. We conclude, based on the lack of statistically significant diagnostic value from our study, and as a conclusion of various studies in the literature, that the main value of these two markers still lies in the fact that they provide greater insight into prognosis of colorectal cancer. Even though our study did not show this, the lack of prognostic value can be traced to the small patient number not to absence of prognostic correlation, as values between controls and patients, as well as between the different classifications of patients, were clearly different in observation, but not so statistically as overall.
If CEA and VEGF levels are to be used for diagnostic purposes, they should be coupled with colonoscopy and biopsy, which remain the golden standards in detection and diagnosis of colorectal carcinoma, and possibly with various stool screening approaches such as fecal occult blood and other potential stool markers [26]. Concomitant high CEA and VEGF levels can potentially select out a subgroup of individuals who may require either earlier or more frequent screening colonoscopy. Until the time comes when there will be one specific marker for colorectal cancer, additional molecular studies on a larger number of patients are needed to validate the above results.
ETHICAL APPROVAL
This article conforms to the ethical standards required by the Lebanese University, and which were followed at all stages of the study.
ACKNOWLEDGEMENTS
The authors would like to thank Dr. Ali Bazarbachi for his critical comments, as well as Ms. Michele P. Zeinieh for her help with the statistical calculations. The study was supported by a grant from the Lebanese University Central Committee for Scientific Research.