- Home
- About Journals
-
Information for Authors/ReviewersEditorial Policies
Publication Fee
Publication Cycle - Process Flowchart
Online Manuscript Submission and Tracking System
Publishing Ethics and Rectitude
Authorship
Author Benefits
Reviewer Guidelines
Guest Editor Guidelines
Peer Review Workflow
Quick Track Option
Copyediting Services
Bentham Open Membership
Bentham Open Advisory Board
Archiving Policies
Fabricating and Stating False Information
Post Publication Discussions and Corrections
Editorial Management
Advertise With Us
Funding Agencies
Rate List
Kudos
General FAQs
Special Fee Waivers and Discounts
- Contact
- Help
- About Us
- Search

The Open Anatomy Journal
(Discontinued)
ISSN: 1877-6094 ― Volume 6, 2014
Clinically Important Anatomical Variation of Cutaneous Branches of Superficial Peroneal Nerve in the Foot
Narendiran K1, Rao Mohandas K.G1, Somayaji S.N.2, Shajan Koshy1, Vincent Rodrigues1
Abstract
A detailed knowledge of the branching patterns and the variations of the cutaneous nerves of the extremities will help to decrease iatrogenic injury to these nerves. A case of abnormal distribution of the superficial peroneal nerve, observed during the routine dissection of the right leg of an 81 year old male cadaver at AIMST University, Kedah, Malaysia is reported here. The nerve after supplying the peroneal muscles of lateral compartment gave a medial dorsal cutaneous branch and a lateral dorsal cutaneous branch. The medial dorsal cutaneous branch descended in front of the middle of the ankle to the dorsum of the foot and supplied the skin of medial side of the great toe, the medial side of the 1st metatarsal region and the 1st web space including the adjacent sides of great and second toes. The lateral dorsal cutaneous branch descended in front of the lateral malleolus to enter the lateral aspect of the dorsum of the foot where it divided into medial and lateral terminal branches to supply adjacent sides of the 2nd, 3rd, 4th and 5th toes. On the other hand, the deep peroneal nerve after supplying the muscles of anterior compartment of leg continued on dorsum of foot without dividing into terminal branches and without supplying the skin of first web space and adjacent sides of great and second toes. It ended by supplying the extensor digitorum brevis muscle. Surgical and clinical significance of this rare variation of the superficial peroneal nerve is discussed and relevant literature is reviewed.
Article Information
Identifiers and Pagination:
Year: 2010Volume: 2
First Page: 1
Last Page: 4
Publisher Id: TOANATJ-2-1
DOI: 10.2174/1877609401002010001
Article History:
Received Date: 8/10/2009Revision Received Date: 26/10/2009
Acceptance Date: 29/10/2009
Electronic publication date: 7/1/2010
Collection year: 2010
open-access license: This is an open access article licensed under the terms of the Creative Commons Attribution Non-Commercial License (http: //creativecommons.org/licenses/by-nc/3.0/ which permits unrestricted, non-commercial use, distribution and reproduction in any medium, provided the work is properly cited.
* Address correspondence to this author at the Faculty of Medicine, AIMST University, Semeling, Bedong- 08100, Kedah Darul Aman, Malaysia, Tel: +60164977261, Fax: +6044298009, E-mail: mohandaskg@gmail.com
| Open Peer Review Details | |||
|---|---|---|---|
| Manuscript submitted on 8-10-2009 |
Original Manuscript | Clinically Important Anatomical Variation of Cutaneous Branches of Superficial Peroneal Nerve in the Foot | |
INTRODUCTION
Normally, the superficial peroneal nerve (SPN) a branch of common peroneal nerve, supplies the peronei longus and brevis and the skin over the greater part of the dorsum of the foot. It passes forward between the peronei and the extensor digitorum longus, pierces the deep fascia at the lower third of the leg, and divides into medial and lateral dorsal cutaneous nerves. In its course between the muscles, the nerve gives off muscular branches to the peroneus longus and peroneus brevis and cutaneous filaments to the skin of the lower part of the leg. The medial dorsal cutaneous nerve passes in front of the ankle-joint, and divides into two dorsal digital branches, one of which supplies the medial side of the great toe, the other, the adjacent side of the second and third toes. It also supplies the skin of the medial side of the foot and ankle and communicates with the saphenous and deep peroneal nerves. The smaller lateral dorsal cutaneous nerve, also called intermediate dorsal cutaneous nerve passes along the lateral part of the dorsum of the foot, and divides into dorsal digital branches, which supply the contiguous sides of the third and fourth, and of the fourth and fifth toes. It also supplies the skin of the lateral side of the foot and ankle, and communicates with the sural nerve. The branches of the SPN supply the skin of the dorsal surfaces of all the toes excepting the lateral side of the little toe, and the adjoining sides of the great and second toes, the former being supplied by the lateral dorsal cutaneous nerve from the sural nerve, and the latter by the medial branch of the deep peroneal nerve [1]. Both branches, especially the lateral are at risk during the placement of portal incisions for arthroscopy [1]. The other terminal branch of common peroneal nerve is deep peroneal nerve. Deep peroneal nerve after supplying the muscles of anterior compartment of leg ends by dividing into medial terminal and lateral terminal branches in front of ankle. Its medial terminal branch accompanies the dorsalis pedis artery along the dorsum of the foot and at the first interosseous space, divides into two dorsal digital nerves which supply the adjacent sides of the great and second toes and first web space [1]. Though the variations in the branches of the SPN are common, the cases of SPN supplying the first web space and the adjacent sides of the great and second toes are rare.
CASE REPORT
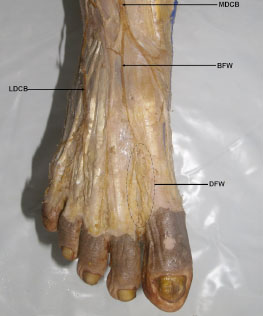
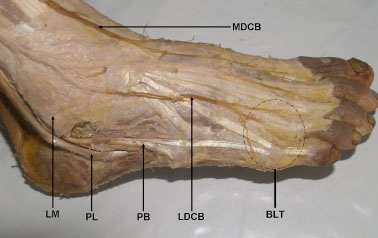
During routine dissection for undergraduate medical students at Department of Anatomy, Faculty of Medicine, AIMST University, Malaysia, unilateral variations in the branches and distribution of SPN were observed in the right leg and foot in 81 year old Malaysian male cadaver. The nerve after supplying the peroneal muscles of lateral compartment gave a medial dorsal cutaneous branch which pierced the deep fascia between the flexor digitorum longus and peroneus longus tendons to emerge in the middle of the anterior compartment of the leg. It then descended in front of the middle of the ankle to the dorsum of the foot and branched to supply the whole of the medial side of the great toe, the medial side of the 1st metatarsal region and the 1st web space including medial side of second toe and lateral side of great toe. The lateral dorsal cutaneous branch continued in the peroneal tunnel in the anterior intermuscular septum and about 2.5cm above the ankle joint it pierced the deep fascia to descend in front of the lateral malleolus to enter the lateral aspect of the dorsum of the foot where it divided into medial and lateral terminal branches to supply adjacent sides of the 2nd, 3rd, 4th, 5th toes lateral side of the little toe (Figs. 1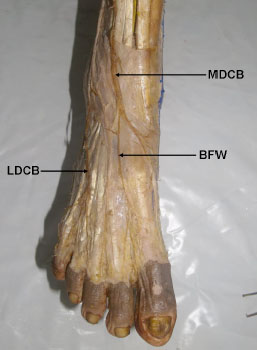 -4
-4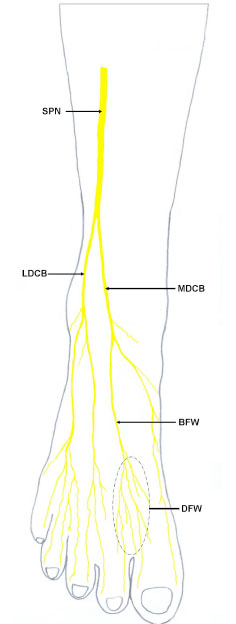 ). On the other hand, the deep peroneal nerve after supplying the muscles of anterior compartment of leg continued on dorsum of foot without dividing into terminal branches. It ended by supplying the extensor digitorum brevis.
). On the other hand, the deep peroneal nerve after supplying the muscles of anterior compartment of leg continued on dorsum of foot without dividing into terminal branches. It ended by supplying the extensor digitorum brevis.
DISCUSSION
Awareness of possible variations in the cutaneous distribution of the leg and foot is essential for clinicians and surgeons. As far as SPN is concerned, many studies have been conducted to assess the possibility of variations. Canella et al. have carried out a sonographic study of SPN and found that the level at which the nerve emerges between the peroneus longus and extensor digitorum longus muscles and the level at which it pierces the crural fascia and becomes subcutaneous were highly variable. They have also reported that it was located in the anterior compartment in 26.7% of the legs and divided before piercing the crural fascia in 6.7% of the legs [2]. In another study of thirty-eight legs of 20 cadavers, Apaydin et al. have found that in 71% of the cases, the SPN coursed entirely within the lateral compartment of the leg (Type I). In 23.7%, the SPN penetrated the anterior intermuscular septum, 12.7 cm inferior to the apex of the head of fibula and coursed in the anterior compartment (Type II). In the remaining 5.3% of the specimens, the SPN had branches both in the anterior and lateral compartments (Type III). It can be noted here that the course of the SPN reported in the present case was different from above mentioned 3 types [3]. A study of SPN carried out in 111 legs has revealed that in 77 (69.4%) specimens, the nerve coursed within the lateral compartment of the leg, while in 18 (16.2%) of the legs, the nerve split and contained branches in both the lateral and anterior compartments. The nerve in 7 (6.3%) legs was found within the intermuscular septum, and in 9 (8.1%) of the specimens, the SPN traveled only within the anterior compartment [4]. Three distinct branch patterns of SPN have been described by Ucerler. In Type 1 (63.3%), the nerve penetrated the crural fascia 8cm proximal to the intermalleolar line and then divided into the intermediate dorsal cutaneous nerve and the medial dorsal cutaneous nerve (classic type). In Type 2 (26.7%), both these branches arose independently from the SPN. In Type 3 (10%), the SPN penetrated the crural fascia about 10cm proximal to the intermalleolar line as a single branch which had a similar course to the medial dorsal cutaneous nerve [5]. Similar findings are reported by Canovas et al. where its emergence was located about 11cm from the lower end of the lateral malleolus and the division of the nerve into the medial dorsal cutaneous and intermediate dorsal cutaneous branches in 29 out of 30 cases [6]. A study conducted by Adkison et al. has revealed that the SPN coursed within the lateral muscle compartment from its origin to its exit through the crural fascia in 73 percent of cases, the nerve had a variable course in the lateral compartment, crossed into the anterior compartment, and passed through the fascia in 14 percent of the legs and it divided in to two branches in both the anterior and the lateral compartment 12 percent of cases [7]. Though there are many reports on the variations in the course, branches and distribution of SPN in the leg, not many reports available on its variations in the foot. A study conducted by Madhavi et al. in 260 Indian feet has showed six patterns of innervation of the toes by the sural and superficial peroneal nerves. They have also reported that the pattern which is usually described in text books [1] was found in only 35.38% of feet [8]. It is relevant here to note that the 6 types of sural and SPN cutaneous distribution explained by them did not include the type reported in the present case where SPN innervates the first web space.
Knowledge of the precise location of SPN and its major branches their possible variations has useful clinical applications. In lateral compartment syndrome, SPN gets entrapped as it penetrates the deep fascia leading to pain over the area of its distribution via an increased intra-compartmental pressure [1, 3]. Fasciotomy is currently the mainstay for surgical treatment for compartment syndrome. Fasciotomy is usually performed either with classical open or minimally invasive techniques including endoscopically assisted or semi blind subcutaneous releases. Incompletely released fascial compartments, soft tissue damage, and neurovascular injury, which include SPN injury, are common complications. Hence knowledge of variations of the SPN with reference to compartmental anatomy of the leg may be useful in fascial release operations [3]. According to Ucerler and Ikiz a detailed knowledge about the SPN and its cutaneous branches may decrease the damage to these nerves during operative procedures near the foot and ankle [5]. The distally-based intermediate dorsal neurocutaneous flap is used in repair of the soft tissue defect in the foot as it has high vascularity. This flap is usually supplied by intermediate dorsal cutaneous branch of SPN which includes the dorsal skin of the second, third and fourth metatarsals and toes [9]. In such surgical procedures possibility the intermediate dorsal cutaneous branch of SPN supplying the first web space as in present case should be kept in mind and that area also should be included in the flap to avoid damaging the twigs supplying that area. Awareness of possible variations in the relationship of the deep peroneal nerve to dorsalis pedis artery on the dorsum of the foot is important for vascular and reconstructive surgeons as it might help in decreasing confusion when considering treatment options like microvascular anastomosis in reconstruction of the leg [10]. However, in the present case the dorsalis pedis artery is related to the medial dorsal cutaneous branch of SPN which supplies the first web space instead of deep peroneal nerve. This variation also has to be kept in mind during vascular and reconstructive surgeries. Such variations also might confuse physician during evaluation of numbness and tingling sensations over the dorsum of the foot in cases of compression syndromes [11]. With these literature reviews, it is evident that a variety of surgical procedures are performed in the vicinity of the SPN, requiring that the surgeon be familiar with its specific anatomical variations.
To conclude, we would like to state that, our findings in above case is one of the rare variations of the SPN. The SPN and its cutaneous branches are at risk during surgical procedures. A detailed knowledge of the branching patterns of the SPN and their variations will help to decrease iatrogenic injury to this nerve.