The Open Arthritis Journal
(Discontinued)
ISSN: 1876-5394 ― Volume 7, 2014
Systemic Lupus Erythematosus and Osteonecrosis: A Comparison of Patients with Single versus Multiple Joint Involvement
Tanaz A. Kermani*, 1, Cynthia S. Crowson2, Kimberly K. Amrami3, Daniel J. Berry 4, Kevin G. Moder*, 1
Abstract
Objective:
The purpose of this study was to determine the clinical and laboratory features associated with osteonecrosis of multiple (>/= 3) joints in systemic lupus erythematosus (SLE).
Methods:
We included all patients with SLE and osteonecrosis evaluated at our institution between January 1, 2000 and June 30, 2006. The patients were divided into three groups based on osteonecrosis of 1 joint, 2 joints and 3 or more joints. Clinical features, laboratory findings and therapies of patients in these groups were compared using Fischer’s exact test and rank sum tests.
Results:
Our study included 4 men and 37 women. Twelve patients (29.3%) had osteonecrosis of 1 joint, 16 patients (39%) had osteonecrosis of 2 joints and 13 patients (31.7%) had osteonecrosis of 3 or more joints. The only clinical feature of SLE significantly associated with osteonecrosis of 3 or more joints was central nervous system (CNS) disease (p = 0.01). The median cumulative and peak corticosteroid doses were similar in all 3 groups (p = 0.70 and p = 0.11 respectively). There were no differences in the frequency of anti-cardiolipin antibodies.
Conclusions:
History of CNS disease was the only variable associated with multiple joint osteonecrosis in patients with SLE. We found no association between corticosteroid doses and multiple joint osteonecrosis.
Article Information
Identifiers and Pagination:
Year: 2010Volume: 3
First Page: 47
Last Page: 52
Publisher Id: TOARTHJ-3-47
DOI: 10.2174/1876539401003010047
Article History:
Received Date: 4/5/2010Revision Received Date: 21/7/2010
Acceptance Date: 25/7/2010
Electronic publication date: 08/09/2010
Collection year: 2010
open-access license: This is an open access article licensed under the terms of the Creative Commons Attribution Non-Commercial License (http://creativecommons.org/licenses/by-nc/3.0/) which permits unrestricted, non-commercial use, distribution and reproduction in any medium, provided the work is properly cited.
* Address correspondence to these authors at the Mayo Clinic, 200 First Street SW, Rochester, MN 55905, USA; Tel: 507-284-2975; Fax: 507-284- 0564; E-mail: kermani.tanaz@mayo.edu Mayo Clinic, 200 First Street SW, Rochester, MN 55905, USA; Tel: 507- 284-1625; Fax: 507-284-0564; E-mail: moder.kg@mayo.edu
| Open Peer Review Details | |||
|---|---|---|---|
| Manuscript submitted on 4-5-2010 |
Original Manuscript | Systemic Lupus Erythematosus and Osteonecrosis: A Comparison of Patients with Single versus Multiple Joint Involvement | |
INTRODUCTION
Osteonecrosis (avascular necrosis) remains a significant cause of morbidity in patients with systemic lupus erythematosus (SLE) [1, 2]. Glucocorticoid use is a major risk factor in the development of this complication [1, 3-8]. Other features which have been associated with development of osteonecrosis in SLE include arthritis [4], central nervous system disease [5, 9, 10], vasculitis [1, 9, 11], hematologic abnormalities [10], renal disease [10], pleural effusions [10] and presence of Raynaud’s phenomenon [1, 9] among others. The role of antiphospholipid antibodies in the development of osteonecrosis remains controversial [11-15]. To date clinical features that predispose to multiple joint osteonecrosis remain poorly understood. To address this question, we conducted a study of all patients with SLE and osteonecrosis evaluated at our institution between January 1, 2000 and June 30, 2006 to determine the clinical and laboratory findings associated with osteonecrosis of multiple joints (≥ 3 joints) in SLE.
PATIENTS AND METHODS
Study Design
This is a retrospective chart review study of all patients with a diagnosis of osteonecrosis and SLE evaluated at our institution between January 1, 2000 and June 30, 2006. All patients provided authorization for review of their medical records. The study was approved by the Institutional Review Board.
Case Retrieval
Using ICD-9 codes for SLE and avascular necrosis or aseptic necrosis bone, all patients with the above diagnoses evaluated at Mayo Clinic, Rochester between January 1, 2000 and June 30, 2006 were identified. All charts were reviewed. Those meeting our criteria for SLE and osteonecrosis were included. Incident and prevalent cases of osteonecrosis were included. Records were reviewed for clinical information. All cases were followed to December 31, 2007.
Case Definitions
Only patients meeting ACR classification criteria for SLE were included. Osteonecrosis was diagnosed by radiographic imaging with plain films and/or MRI.
Exclusion Criteria
Patients were excluded if they did not meet ACR classification criteria for SLE or did not have radiographic evidence of osteonecrosis.
Data Collection
A standardized data collection form was used. Data on age at diagnosis of SLE, age at diagnosis of osteonecrosis, duration of SLE and gender were collected. Clinical manifestations of SLE and symptoms at presentation of osteonecrosis were documented. Laboratory information collected included autoantibodies, antiphospholipid antibodies (if tested), total cholesterol, high-density lipoprotein and low-density lipoprotein. Use of cytotoxic medications (azathioprine, mycophenolate mofetil, cyclophosphamide, methotrexate or leflunomide) was documented. We collected information on corticosteroid doses from diagnosis of SLE to the date of last osteonecrosis event. Radiologic reports were reviewed for distribution, location and number of joints affected by osteonecrosis. If a patient had prior surgery for osteonecrosis that was well documented in their medical records, the replaced joints were also included in the number of joints affected by osteonecrosis. Systemic Lupus International Collaborating Clinics/American College of Rheumatology (SLICC/ACR) Damage Index was calculated at the last visit to assess cumulative damage in these patients [16].
Statistical Analysis
The patients were subdivided into three groups based on the number of joints affected by osteonecrosis as follows: Group A had involvement of only 1 joint, Group B had involvement of 2 joints and Group C had 3 or more joints affected by osteonecrosis. Fisher’s exact test was used for statistical analysis of clinical features between the three groups and the Kruskal-Wallis rank sum test was used to compare continuous measures across the 3 groups. Cumulative corticosteroid doses were estimated by adding the daily doses across the follow-up time. Sensitivity analysis were used to examine the influence on the estimates of cumulative dose and the differences between groups using various assumptions regarding dosage changes during tapering and during brief periods when steroid dosage was not available for a few patients. In addition, the cumulative corticosteroid doses were estimated both including and excluding intravenous pulse steroids.
RESULTS
One hundred and sixteen patients were evaluated at our institution for osteonecrosis and SLE between the dates of interest. Seventy-five patients were excluded for the following reasons: 26 (22.4%) did not meet 4 or more classification criteria for SLE, 9 patients (7.8%) did not have information in the medical records to confirm a diagnosis of SLE, 4 (1%) had an alternate diagnosis (dermatomyositis, p-ANCA vasculitis, scleroderma and mixed connective tissue disease), 14 patients (12.1%) did not have radiographic evidence of osteonecrosis, and 22 patients (19%) had a “history” of osteonecrosis. Therefore, only 41 patients (35.3%) met our entry criteria. Thirty-seven (90.2%) were women and 4 (9.8%) were men. Twenty-five patients (61%) had a first diagnosis of AVN made between January 1, 2000 and June 31, 2006.
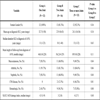
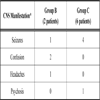
Twelve patients (29.3%) had osteonecrosis of 1 joint, 16 patients (39%) had 2 joints affected and 13 patients (31.7%) had involvement of 3 or more joints. Mean age at diagnosis of SLE and mean duration of SLE to diagnosis of osteonecrosis was similar across all three groups (Table 1). Pain was the presenting symptom that led to diagnosis of osteonecrosis in all cases. The clinical manifestations of SLE in all 41 patients were as follows: malar rash in 17 (41.5%); mucositis in 5 (12.2%); photosensitivity in 5 (12.2%); arthritis in 35 (85.4%); serositis in 14 (34.1%); nephritis in 27 (65.9%); CNS disease in 8 (19.5%) and hematologic manifestations in 18 (43.9%). Comparison of SLE manifestations in the 41 patients based on the number of joints affected found CNS disease was the only statistically significant clinical feature of SLE that was associated with multiple joint involvement (p=0.01) (Table 1). The CNS manifestations of these 8 patients are summarized in Table 2.
We divided patients into three groups based on number of joints affected by osteonecrosis. However, given the uncertainty of whether Group B is more similar to Group A (i.e. later stage of disease) or to Group C (precursor to involvement of more joints), we also conducted analyses combining Groups A + B and comparing to Group C and combining groups B + C and comparing to Group A (data not shown). Combining Groups A + B and comparing to Group C, we continued to observe a statistically significant association between presence of CNS disease and osteonecrosis of three or more joints (p=0.01). Finally, combining Groups B + C and comparing to Group A, a statistically significant relationship was noted between hematologic manifestations and involvement of 2 or more joints (p= 0.04).
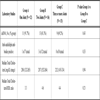
Pertinent laboratory findings for the 3 groups are summarized in Table 3. All patients had a positive anti-nuclear antibody. Anti-double stranded DNA antibodies were next most commonly observed antibody in all three groups. Anti-cardiolipin antibodies were checked in 27 patients (65.9%). Only 8 subjects in this study were screened for lupus anticoagulant and given the small numbers, these results were not reported.
Median peak corticosteroid doses and median cumulative corticosteroid doses were similar across all three groups (Table 4). There was a trend toward more cyclophosphamide use and osteonecrosis of 3 or more joints but this did not reach statistical significance (p=0.09). There was no difference between the 3 groups in use of mycophenolate mofetil, leflunomide or methotrexate. History of azathioprine use was more common in the group with 1 joint AVN compared to the other groups (p=0.05, Table 4).
Osteonecrosis was diagnosed by plain films in 20 patients (48.8%), a combination of plain films and MRI in 14 patients (34.1%), plain films and bone scan in 1 patient (2.4%) and MRI only in 6 patients (14.6%). Nine of 12 patients (75%) from Group A also had imaging of the asymptomatic contralateral joint (7 patients with x-rays, 1 patient with CT and 1 patient with MRI), which did not show involvement from osteonecrosis. In Group B, 9 patients (56.3%) were incidentally noted to have osteonecrosis of the asymptomatic, contralateral joint by imaging; MRI in 5 patients and x-rays in 4 patients.
Total number of joints affected by osteonecrosis was 98. Hips were the most commonly affected joint (55.1% joints involved) followed by knees (34.7% joints involved), ankles (6.1% joints involved) and shoulders (3.1% joints involved). Wrist disease was noted in 1 patient. Fifteen patients from Group B had bilateral disease and all patients in Group C had bilateral disease in at least one joint area affected. Bilateral disease was present in 23 patients with hip involvement, 13 patients with knee osteonecrosis, 2 patients with ankle disease and 1 patient with shoulder involvement.
Therapy and Outcomes
Twenty-five patients (61%) in this study underwent surgery for osteonecrosis. Two patients (16.7%) from Group A required surgery. Both patients had unilateral total hip arthroplasties. In Group B, 11 patients (68.8%) underwent surgery, which were comprised of unilateral hip arthroplasties in 5 patients, bilateral hip arthroplasties in 3 patients, unilateral knee arthroplasties in 2 patients and shoulder arthroplasty in 1 patient. Twelve patients in Group C underwent surgery for osteonecrosis. Surgical procedures included unilateral total hip arthroplasties in 2 patients, bilateral total hip arthroplasties in 5 patients, bilateral hip decompression surgeries in 2 patients, unilateral total knee arthroplasty in 2 patients, bilateral total knee arthroplasty in 1 patient, tibial osteotomy in 1 patient and shoulder hemiarthroplasty in 1 patient.
DISCUSSION
Osteonecrosis is a known complication of SLE with corticosteroid use being a primary risk factor. Prevalence estimates of osteonecrosis in SLE range from 3-30% [17]. While glucocorticoid use remains a major risk factor for development of this complication, multiple other factors have also been associated with development of osteonecrosis in SLE. In this study, we compared patients with osteonecrosis of 1, 2 and 3 or more joints to characterize the clinical and laboratory features associated with osteonecrosis of 3 or more joints.
We divided the 41 patients identified into 3 groups based on the number of joints affected by osteonecrosis. This decision was mainly due to difficulty classifying 16 patients with 2 joints involved (Group B). Fifteen patients in this group had bilateral joint involvement. Therefore, it remains unclear if Group B represents a later stage of patients with osteonecrosis of 1 joint, or, an earlier stage of disease and is a precursor to multiple joint involvement. Furthermore, osteonecrosis of a contralateral asymptomatic joint was incidentally diagnosed by imaging studies in 9 of 16 patients in Group B. While the primary presenting symptom of osteonecrosis is pain, asymptomatic osteonecrosis in SLE has been described [18]. Asymptomatic osteonecrosis has been reported in several studies using prospective MRI imaging [12, 19-21]. In a prospective study of 66 patients with SLE and no symptoms referable to the hip, the investigators found asymptomatic osteonecrosis in 8 patients (12%) [21]. In another prospective study using MRI of the hips, asymptomatic osteonecrosis was noted in 15 of 45 (33%) patients studied [19]. Five of 15 patients in this study, later developed symptoms 2 to 4 years after MRI changes were first noted [19]. Finally, in an MRI study of the lower limbs in 40 patients with SLE, 13 patients had 123 MRI-detected osteonecrosis lesions [12]. Of these, clinically silent lesions were present in 53% of hips, 84% of knees and 75% of ankles [12]. Therefore, there are obvious challenges when studying osteonecrosis in SLE patients since lesions may be radiographically undetectable or asymptomatic. Despite this, we are reasonably confident in the classification of patients with involvement of only 1 joint since in 75% of cases in Group A, the contralateral asymptomatic joint had also been imaged and findings of osteonecrosis were absent. However, 7 of the 9 patients with contralateral joint imaging had x-rays performed which may have affected the sensitivity with which asymptomatic contralateral disease is detected.
Thirteen patients (31.7%) in this series had osteonecrosis of 3 or more joints (multifocal osteonecrosis). In two large studies of osteonecrosis, multifocal involvement was seen in approximately 3% patients and is likely an underestimation since not all joints are systematically imaged [22, 23]. Additionally, among patients with multifocal osteonecrosis, between 38-41% of patients have SLE [22, 23]. Hips remain the most commonly affected joint by osteonecrosis (non-multifocal or multifocal). The distribution of joint involvement noted in our study is similar to that of other studies with hips being the most commonly affected, followed by knees [17]. Bilateral involvement was common and was noted in 15 patients from Group B. Additionally, all patients in the group with 3 or more joints affected with osteonecrosis had bilateral involvement of at least one joint area.
The mean duration of SLE at development of osteonecrosis was similar across the three groups. History of CNS disease was the only clinical feature of SLE that correlated with osteonecrosis of 3 or more joints. Three prior studies have found an association between CNS disease and osteonecrosis in SLE [5, 9, 10]. In the study by Cozen and Wallace comparing 26 SLE patients with osteonecrosis to 462 SLE patients without osteonecrosis, cerebritis was present in 26.3% of patients with osteonecrosis compared to only 9.7% of patients without osteonecrosis (p = 0.01) [10]. In a cohort study comparing 38 patients with SLE and osteonecrosis to 143 patients with SLE without osteonecrosis, presence of CNS disease was more common in patients with osteonecrosis (39% patients) compared to 14% patients without osteonecrosis, p<0.001) [5]. The authors concluded that the higher prevalence of CNS disease reflected the need for higher initial corticosteroid dose. We hypothesized that the association of CNS disease with multiple joint involvement from osteonecrosis was related to more serious disease and therefore more aggressive therapy for SLE. However, we were unable to find any differences in the 3 groups with respect to cumulative or peak corticosteroid doses. Corticosteroid use in SLE has been implicated as a risk factor for osteonecrosis in several studies [1, 4, 5, 8, 11, 24]. Highest glucocorticoid dose [4, 5, 8, 11, 24], cumulative corticosteroid dose [4] and duration of corticosteroid treatment [24] have all been evaluated and associated with osteonecrosis. Previous studies have examined corticosteroid treatment and development of osteonecrosis. In this study, we were evaluating corticosteroid treatment with respect to number of joints affected by osteonecrosis. While peak and cumulative corticosteroids doses were not different between the three groups, all patients in this study had received treatment with corticosteroids. We also failed to find an association with cytotoxic medication use (cyclophosphamide or azathioprine) when analyzing across the 3 groups. However, when Groups A and B were combined and compared to Group C, we did find a greater proportion of patients in Group C received cyclophosphamide (25% from Groups A and B compared to 61.5% from Group C, p = 0.04). Cytotoxic medication use has been associated with osteonecrosis in SLE. In a study by Mok et al. additional immunosuppression with cyclophosphamide was more common in patients with osteonecrosis compared to those without [5]. Gladman et al. also found a statistically significant difference in cytotoxic medication use among patients with SLE and osteonecrosis compared to SLE patients without osteonecrosis [4]. In a recent nested matched case-control study, cytotoxic medication use (cyclophosphamide and/or azathioprine) was associated with development of symptomatic osteonecrosis [24]. Based on our findings, there may have been an association between cyclophosphamide use and osteonecrosis of 3 or more joints when comparing Groups A+B to Group C. However, there was no association between multiple joint osteonecrosis and azathioprine. Furthermore, in our study, a larger proportion of patients in the Group A were on azathioprine compared to the other two groups. The reason for this asymmetry in azathioprine exposure is unclear since apart from CNS disease, the clinical manifestations between the three groups were similar. This may be related to the small numbers in our study. Alternatively, while azathioprine may be a risk factor for development of osteonecrosis, it may not play a role in the number of sites involved.
We did not find an association of specific autoantibodies and the development of osteonecrosis in multiple joints. In a previous study, of 7 patients with SLE who developed osteonecrosis, concurrent anti-Ro (SS-A) antibodies and anti-RNP antibodies were noted in 3 patients while another 2 patients with osteonecrosis had antibodies to topoisomerase I [25]. The role of antiphospholipid antibodies remains controversial. Based on the numbers available, there was no association between the presence of anti-phospholipid antibodies and osteonecrosis of more than 1 joint. However, not all patients in our study were tested. The prevalence of positive antiphospholipid antibodies in our study (15%) is lower than that reported in other series of SLE patients with osteonecrosis [1, 14, 24-26] In a study comparing patients with osteonecrosis to those without osteonecrosis, an abrupt change in ratio of total cholesterol at one month was associated with development of osteonecrosis [19]. A clinical trial comparing atorvastatin to placebo in reducing incidence of osteonecrosis in steroid-treated lupus has been initiated [27]. The total cholesterol and total cholesterol/high-density lipoprotein (HDL) ratio was similar for all three groups.
Finally, 25 patients (60.1%) in this study underwent surgery for osteonecrosis. While only 2 patients (17%) from Group A underwent surgery,11 patients (69%) in Group B and 12 patients (92%) in Group C had surgery of at least one affected joint. The difference in surgical interventions between the groups may be related to higher number of affected joints in Groups B and C. Several patients in Group C underwent surgical intervention of more than one affected joint. Alternatively, the low percentage of procedures in group A may be a reflection of the shorter duration of follow-up.
There are several limitations to this study. This study was conducted at a tertiary care facility. It is estimated that approximately 200 patients with SLE are evaluated at our center each year. However, the SLE patient population seen at Mayo Clinic is predominantly Caucasian and the sample size of this study was small. Additionally, this was a retrospective chart review and therefore we were only able to abstract information available in the medical record. The median length of follow-up differed between the three groups although this was not statistically significant. The group with single joint involvement had the shortest follow-up time. Therefore, it is possible that the diagnosis of osteonecrosis in 2 or more joints was due to longer follow-up interval in the group with 3 or more joints rather than differences between the 3 groups. However, the majority of patients with multiple joint involvement (23 of 29, 79%) had osteonecrosis in more than one joint simultaneously suggesting that all our findings are unlikely due to duration of follow-up alone. Furthermore, SLICC/ACR damage index calculated at the last visit was similar across all 3 groups. In a minority of cases only symptomatic joints were imaged. For most patients, information was also available for the asymptomatic contralateral joint. However, some patients underwent only x-rays of the contralateral joint while other patients had more sensitive imaging modalities like MRI performed for the asymptomatic contralateral joint. Additionally, even for cases diagnosed with osteonecrosis, imaging modalities varied with some cases diagnosed by MRI and others by plain radiographs.
CONCLUSIONS
In summary, our study found an association between history of CNS involvement in SLE and multiple joint osteonecrosis. We also found an association of cyclophosphamide use and multiple joint osteonecrosis. There was no association between peak or cumulative corticosteroid doses and the number of joints affected by osteonecrosis. The association of CNS disease and cyclophosphamide use suggests the SLE patients with multiple joint involvement have more severe systemic disease.
SOURCES OF SUPPORT
Mayo Foundation.