- Home
- About Journals
-
Information for Authors/ReviewersEditorial Policies
Publication Fee
Publication Cycle - Process Flowchart
Online Manuscript Submission and Tracking System
Publishing Ethics and Rectitude
Authorship
Author Benefits
Reviewer Guidelines
Guest Editor Guidelines
Peer Review Workflow
Quick Track Option
Copyediting Services
Bentham Open Membership
Bentham Open Advisory Board
Archiving Policies
Fabricating and Stating False Information
Post Publication Discussions and Corrections
Editorial Management
Advertise With Us
Funding Agencies
Rate List
Kudos
General FAQs
Special Fee Waivers and Discounts
- Contact
- Help
- About Us
- Search

The Open Clinical Trials Journal
(Discontinued)
ISSN: 1876-8210 ― Volume 4, 2013
Antibiotics and Micronutritional Blend to Enhance Fertility Potential in Male Having Abnormal Semen Parameters
Mosammat Rashida Begum*, 1, David Miller2, M.A. Salam3, Ehsan Quadir4, Mosammat Sahina Begum5, Farzana Khan5, Zahid Hassan Bhuiyan6
Abstract
Objective:
Objective of this study was to explore the effect of empirical antibiotics and micro nutritional blends in infertile men having idiopathic oligospermia, asthenospermia and oligoasthenospermia
Materials and Methods:
This prospective cross sectional study was undertaken in a tertiary level infertility care unit of Dhaka between September 2005 and December 2007. Two hundred and seven oligo, astheno and oligoasthenospermic patients were the target population for this study. Thorough infertility evaluation was done to identify idiopathic oligo, astheno and oligoasthenospermia. Female partners were also evaluated to exclude bilateral tubal blockage, pelvic inflammatory diseases, endometriosis, uterine pathology and resistant PCOS. Male partners were divided into three groups for I) Antibiotics and micronutrients, II) only micronutrients and III) no intervention as control. Treatment was continued for three months. Semen analysis was repeated at the end of two and three months. Main outcome measures were improvement of semen parameters and pregnancy rate.
Results:
Before treatment all patients’ characteristics were comparable. After treatment there was significant improvement both in count and motility in groups I and II p <0.05. In group III where there was no intervention there was no improvement of semen parameters p >0.05. Six patients (8.70%) from group I and 12 patients (17.29%) from group II got pregnant within 6 months of observation. No one got pregnant from group III.
Conclusion:
Empirical use of antibiotics and micronutrients in idiopathic oligo, astheno and oligoasthenospemia can improve sperm quantity and quality and aid a couple in achieving pregnancy.
Article Information
Identifiers and Pagination:
Year: 2009Volume: 1
First Page: 7
Last Page: 12
Publisher Id: TOCTJ-1-7
DOI: 10.2174/1876821000901010007
Article History:
Received Date: 31/3/2008Revision Received Date: 14/10/2009
Acceptance Date: 21/10/2009
Electronic publication date: 16/12/2009
Collection year: 2009
open-access license: This is an open access article licensed under the terms of the Creative Commons Attribution Non-Commercial License (http: //creativecommons.org/licenses/by-nc/3.0/) which permits unrestricted, non-commercial use, distribution and reproduction in any medium, provided the work is properly cited.
* Address correspondence to this author at the 2/4 Block “F”, Monjuri, Flat A-1, Lalmatia, Dhaka-1207, Bangladesh; E-mail: rashida_icrc@yahoo.com
| Open Peer Review Details | |||
|---|---|---|---|
| Manuscript submitted on 31-3-2008 |
Original Manuscript | Antibiotics and Micronutritional Blend to Enhance Fertility Potential in Male Having Abnormal Semen Parameters | |
INTRODUCTION
There is a growing body of scientific evidence supporting the idea that sperm counts have declined considerably over the last 50 years. The total sperm count as well as sperm quality of the general male population has been deteriorating over the past few decades. This downward trend in sperm count has led to speculation that environmental, dietary or lifestyle changes in recent decades may be interfering with a man’s ability to manufacture sperm. About 90% of male factor infertility is idiopathic with no identifiable cause. Only a minority of affected males has a definite detectable abnormality related to infertility. Associated factors are, endocrine disease 1-3% [1], antisperm antibodies 3-13% [2], varicocele 25.4% [3], genetic cause 10-15%.
Deterioration of semen parameters may be due to exposure (s) to environmental toxicants that alter the reproductive hormones, spermatogenesis or sperm function. The most widely studied evidence of potential environmental reproductive hazards is that sperm counts have declined in certain industrialized countries [4-7]. Various chemicals have been implicated as reproductive toxicants. A number of these chemicals categorized as air pollutants are present in the blood, urine and semen of exposed men and many affect sperm quality. Air pollution may adversely affect semen quality [8-12].
Nutritional and lifestyle changes can improve semen parameters. Reproductive organs are highly susceptible to free radicals or oxidative damage from environmental toxins like pesticides, insecticides and heavy metals. A balanced nutritional diet and nutritional supplements with high antioxidant content can help reverse some of the oxidative damage from environmental toxins and natural aging. Different micronutrients like Vit C, Vit B12, Vit E, Arginine, Carnitine, Zinc and Selenium have specific roles in increasing sperm count and improving function [13-16].
Male accessory gland infection (MAGI) is associated with abnormal semen parameters. Both chronic and acute infection of the accessory sex glands result in diminished secretory function. Motility is affected by membrane damage by reactive oxygen species generated by white blood cells. It is estimated that 28% to 78% of infertile men have evidence of a chlamydial infection [17]. Chlamydial infection is associated with low sperm count and reduced motility. Sometimes the infection remained completely unrecognized. So the empirical use of antibiotics may sometimes be helpful for unrecognized chlamydial infection.
Considering the positive effects of micronutrients on sperm motility and count a mixture of micronutrients can be applied to reverse sperm parameters. On the basis of published scientific literature on individual nutritional components that benefit fertility, we wanted to use the different components as a blend for oligoasthenospermia. Subclinical epidedymities, which can not be diagnosed by culture, cause oxidative damage of sperm. So empirical antibiotics can also help to maintain sperm function. The purpose of this study is to explore the effect of a micro nutritional blends and empirical antibiotics in infertile men having idiopathic oligospermia, asthenospermia and oligoasthenospermia.
MATERIALS AND METHODS
This experimental study was conducted in Dhaka Medical College Hospital and Infertility Care and Research Centre (a tertiary level infertility care unit), Dhaka, Bangladesh from September 2005 to December 2007. The study protocol was approved by the institutional review board of Dhaka Medical College, Bangladesh. Informed consent was taken from all patients.
Two hundred and seven infertile male patients who attended the Infertility Care and Research Centre were the target population for this study. Semen analysis was performed on two occasions at 8 week interval and at least one of analysis was at the Infertility Care and Research Centre. Detailed personal history was taken regarding occupation, lifestyle, and personal habit of smoking, alcoholism and drug history. Genital tract infection was evaluated by semen culture and sensitivity and chlamydial antibody testing. Antisperm antibody was tested both in sera and sperm surface. General and endocrinological diseases were identified by clinical examination, hormone analysis, CBC, blood sugar and VRDL testing. Thorough physical examination was done by an andrologist. If any specific cause of oligospermia, asthenospermia or oligoasthenos-permia was identified it was excluded from the study. Cases having high FSH level, which indicates compromised testicular function were excluded. Smokers and patients having history of taking any drugs or alcohol were excluded. Fertility assessment of the female partner was done. Uterine pathology, endometriosis, bilateral tubal block, history of pelvic inflammatory diseases, resistant PCOS or any patient who failed to ovulate even with controlled ovarian hyperstimulation were excluded.
All patients were advised to avoid hot environments, diary products, non-organically grown products and to consume organic fruits and vegetables during the study period.
The seminological inclusion criteria were normal appearance, consistency, liquefaction, volume and pH, sperm concentration <20x106/ml, total motility <40%, forward motility<20% and abnormal sperm <70%. Selected patients were divided into three groups by lottery.
Group I
Group I was treated by antibiotics Doxicycline 100mg bd for 1 month followed by micronutrients for 3 months.
Vit C-1 gm daily
Vit E- 800 IU daily
Vit B12-1000 mcg daily
Zinc-120 mg daily
Carnitine-2.64 gm daily
Group II
Group II was treated with the same micronutrients only for 3 months.
Group III
Group III were advised about life style changes only; no medication was given, not even placebo as vitamins are usually used for placebo.
All were advised to repeat semen analysis on 2 occasions, at the end of 2nd and 3rd months. Analysis was done by neuber counting chamber. All analyses were done by the same observer. Motility was assessed as percentage of
- Rapid forward progression
- Slow forward progression
- Non progressive
- Non-motile.
After improvement of semen parameters anovulatory female partners were treated by ovulation inducing agents with monitoring of ovulation. Vit E, Vit C and Carnitine were continued till pregnancy or for another 6 months to match wife’s 6 ovulatory cycles.
Final outcome measures were improvement in sperm count and motility and pregnancy rate.
Data Analysis
Data were analyzed by SPSS software. Mean ± SD, students’ t test and one way ANOVA were performed for test of significance. A value of <0.05 was considered significant
RESULTS
Two hundred and seven patients were recruited for three management options. Patients were selected on the basis of exclusion of all patients having any specific cause of oligoasthenospermia. All recruited patients were free from any medical diseases.
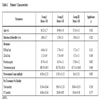
All three groups had similar characteristics regarding age, duration of infertility, basal hormone levels, pretreatment count and motility (Table 1).
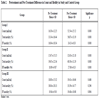
Table 2 shows the pretreatment and post-treatment difference in count and motility. In group I and II (study group) there is a significant difference in count with treatment, p<0.001. There is a 210% and 108% increment in group I and group II respectively. But control group (group III), did not show any change in count, p>0.05. When it was analyzed in individual group it shows a significant change in motility among treatment groups. In both treatment groups both total and fast forward motility was increased significantly, p<0.001. Total motility increment was 70% and 52% and fast forward motility was 50% and 49% in group I and II respectively. But in group III there was no change in motility percentage, p>0.05.
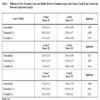
Group I was treated by antibiotics and micronutrients and group II were treated by micronutrients only. So post-intervention count and motility were compared between the individual groups and Table 3 shows that count was increased much more in group I and there is a significant difference between group I and control p<0.001. There is also a significant change between group II and control p<0.05. Although count was increased in both treatment groups but the increment was significantly higher in group I p<0.05.
Table 3 shows motility compared between treatment and control groups. When group I was compared with control, there was a significant change in total motility (p<0.001) but not in fast-forward motility (>0.05). On the other hand motility increment was significant in group II in comparison to control for both total (p<0.001) and fast forward (p<0.05). Among the two treatment groups there was no significant difference in motility increment (p>0.05).
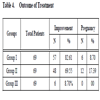
Table 4 shows the improvement of semen parameters after treatment or after just passage of time. In groups I and II there was 82.61% and 69.55% improvement respectively after treatment in terms of count and motility. In group III though there was no intervention, 8.70% show change of seminal parameters. Six patients (8.70%) from group I and 12 patients (17.29%) from group II got pregnant within 6 months of observation. No one got pregnant from group III. Though improvement was better in group I, pregnancy rate was higher in group II.
DISCUSSION
Most cases of male infertility are due to an abnormal sperm count or low sperm motility. Low sperm count or motility dramatically reduces the chance of sperm reaching the egg. In about 10% of the cases of low sperm count the cause can be identified and treated medically.
Nutritional and life style changes increase chances of conception. In known cases fertility potential can be improved by avoiding smoking, caffeine, drugs, alcohol consumption and stress, which are related to infertility. Reproductive organs are highly susceptible to free radicals or oxidative damage from environmental toxicants like pesticides, insecticides, lead, radiation and heavy metals and natural aging. In idiopathic oligospermia and asthenospermia, where there is no specific reason for life style changes, a simple balanced nutritional diet and nutritional supplements with antioxidants can help reverse some of the oxidative damage from environmental toxins and natural aging.
In men certain nutrients are essential for formation of healthy sperm. Micronutrients like vitamin C, vitamin E, L carnitine, zinc, vitamin B complex are critical nutrients in the male reproductive system for proper hormone metabolism, sperm formation and motility. Although high intake of fruits, vegetables, whole grains and nuts are important, supplements are also needed to get sufficient amounts of these nutrients for noticeable effects on sperm quality.
In some cases bacterial infection may cause oxidative damage but infection remains unrecognized even by culture and sensitivity. So empirical antibiotic in some cases may reduce oxidative damage of sperm and improve semen quality. In the present study the two treatment groups showed a marked increment of count and motility of sperm in comparison to the no treatment group. Among two-treatment groups, group I, which included antibiotics showed more improvement than micronutrients alone.
Free radical or oxidative damage to sperm is thought to be responsible for many cases of idiopathic oligospermia. This is causally related to the ability of male germ cells to generate reactive oxygen metabolites. When produced in low levels such metabolites are thought to enhance sperm function by DNA compaction and promoting the induction of sperm capacitation. When produced in excessive amounts, the same metabolites stimulate DNA fragmentation and a loss of sperm function associated with peroxidative damage to the sperm plasma membrane. Use of antioxidants has been shown to be very important in protecting the sperm against damage. Different studies showed the positive effect of direct antioxidants in improving sperm count and motility [18-26]. In a double blind placebo controlled study of 110 men with subnormal sperm activity, treatment with 100IU of vitamin E daily resulted in improved sperm activity [20]. However, a small double blind trial found no benefit from high doses of vitamin E and C [27]. Some studies showed positive effect of using vitamin E in high doses (600 and 800 IU daily) [28,29]. In our study we found profound positive effects but we can not isolate the drug effects as we used in combination.
Vitamin B12 deficiency in men can lead to reduced sperm counts and lowered sperm motility. For this reason B12 supplements have been trialed for improving fertility in men with abnormal sperm production. In one double blind study of 375 infertile men B12 supplementation produced no benefit as a whole [30]. However, weak evidence suggests that B12 supplements may improve sperm count and motility in poor semen parameters [21].
Different double blind placebo controlled trials have demonstrated positive effects of oral L-carnitine and zinc to improve sperm function [22-24, 31-33]. A double blind placebo controlled study showed the significant improvement of sperm count and motility by administration of zinc in infertile men [34]. In the present study zinc and carnitine are also used along with vitamins and the effect of a combination drug is significant.
In the group treated with micronutrients only or by antibiotics plus micronutrients, increase in count and motility is significant in comparison to untreated group (Table 2). As individual micronutrient has positive effect on sperm count and motility this combined effect should be more beneficial. A number of studies have evaluated the benefits of antioxidants for male infertility, which are consistent with the present study also [18-26].
In-group I, 82.61% of patients showed improvement, which is much higher than improvement shown by group II, 69.55%. Pregnancy rate was lower in group I than in group II despite a greater improvement in count and motility. As pregnancy is the combined result of male and female parameters so improvement of semen parameters is not the sole indicator of a couples’ fertility potential.
Microdeletion of the section of the Y chromosome may be detected in 3% to 10% of oligospermic men with normal karyotype [35,36], which can not be detected by karyotyping but can be identified with sequenced –tagged site probes along entire length of the Y chromosome. Most deletions occur in AZF regions of the long arm of Y chromosome that contains multiple genes important for spermatogenesis. The limitation of the present study is that we could not do the genetic testing and we may miss chromosomal defects if there is any. Few patients in this study did not respond to treatment at all; genetic problem can not be ignored in those cases.
Treatment of male infertility is a challenge for fertility specialists. Various nutritional strategies have been presented, which have a beneficial impact on sperm count, motility and ultimately fertility. For males with idiopathic infertility, dietary supplementation with a combination of well tolerated, clinically efficacious and non-invasive vitamins and vitamin-like agents (vit C, E, B12, carnitine and zinc) provide an alternative pharmacological therapy, which can improve sperm quantity and quality and aid a couple in achieving pregnancy.