- Home
- About Journals
-
Information for Authors/ReviewersEditorial Policies
Publication Fee
Publication Cycle - Process Flowchart
Online Manuscript Submission and Tracking System
Publishing Ethics and Rectitude
Authorship
Author Benefits
Reviewer Guidelines
Guest Editor Guidelines
Peer Review Workflow
Quick Track Option
Copyediting Services
Bentham Open Membership
Bentham Open Advisory Board
Archiving Policies
Fabricating and Stating False Information
Post Publication Discussions and Corrections
Editorial Management
Advertise With Us
Funding Agencies
Rate List
Kudos
General FAQs
Special Fee Waivers and Discounts
- Contact
- Help
- About Us
- Search

The Open Conference Proceedings Journal
(Biological Sciences, Chemical Sciences, Physical Sciences, Medicine, Engineering & Technology)
(Discontinued)
ISSN: 2210-2892 ― Volume 10, 2020
Computer Aided Formulation and Characterization of Propranolol Hcl Buccal Tablet Using Polymeric Blend
Sana Hanif1, Nadeem Irfan2, Zeeshan Danish2, *, Nisaar Hussain3, Muhammad Ali1, Bushra Nasir3, Javed Iqbal1, Hamid Saeed3, Rubina Ali1, Zikria Saleem2
Abstract
The current study was aimed to formulate a continuous release mucoadhesive buccal tablet containing propranolol HCl. The type and quantities of polymers as well as method of compression were set in a preliminary study (F1-F13). Direct compression method was employed in the main study (F14-F24) using Carbopol® 934P (CP), ethylcellulose (EC), sodium alginate (SA), hydroxypropyl methylcellulose (HPMC k4M) and carboxymethylcellulose (CMC) as mucoadhesive polymers and were tested for physicochemical tests i.e. swellability, surface pH, mucoadhesive time, mucoadhesive strength, in vitro release etc. Results obtained from the study were optimized using NeuralPower® 3.1, an artificial intelligence approach. Against the desirability of physico-chemical parameters, the software optimized the ingredients as HPMC (150mg), CMC (25mg), CP (20mg) and EC (20mg). Outcome revealed that HPMC primarily contributed to the physicochemical properties of mucoadhesive formulation. To compare prediction, optimized ingredients were formulated (F25) and tested. The swellability index of confirmation formulation (F25) was 102% at 6 h. As predicted, similar release pattern was of F25 was obtained as 26% (0.5h), 34% (1h), 40% (2h), 45% (3h), 50% (4h), 62% (5h), 76% (6h), 85% (7h) and 97% (8h) respectively. For release kinetics, DD solver® suggested the release of the drug to be non-Fickian.
Article Information
Identifiers and Pagination:
Year: 2017Volume: 8
First Page: 1
Last Page: 13
Publisher Id: TOPROCJ-8-1
DOI: 10.2174/2210289201708011001
Article History:
Received Date: 11/10/2015Revision Received Date: 29/09/2016
Acceptance Date: 17/10/2016
Electronic publication date: 12/01/2017
Collection year: 2017
open-access license: This is an open access article licensed under the terms of the Creative Commons Attribution-Non-Commercial 4.0 International Public License (CC BY-NC 4.0) (https://creativecommons.org/licenses/by-nc/4.0/legalcode), which permits unrestricted, non-commercial use, distribution and reproduction in any medium, provided the work is properly cited.
* Address correspondence to this author at the University College of Pharmacy, University of the Punjab, Lahore, Pakistan; Tel: +92-426169211, +92321-4041222; E-mail: pfarmacist@hotmail.com
| Open Peer Review Details | |||
|---|---|---|---|
| Manuscript submitted on 11-10-2015 |
Original Manuscript | Computer Aided Formulation and Characterization of Propranolol Hcl Buccal Tablet Using Polymeric Blend | |
1. INTRODUCTION
The oral route of drug administration is preferred over other routes because of diverse benefits [1Varadarajulu, S.; Tamhane, A.; Drelichman, E.R. Patient perception of natural orifice transluminal endoscopic surgery as a technique for cholecystectomy. Gastrointest. Endosc., 2008, 67(6), 854-860.
[http://dx.doi.org/10.1016/j.gie.2007.09.053] [PMID: 18355816] ]. The harsh environment to which an oral delivery system is exposed to after administration is a major drawback for drug delivery system e.g. acidity, enzymatic action etc. These drawbacks are the extreme pH variations, gastrointestinal enzymes and others [2Marschütz, M.K.; Bernkop-Schnürch, A. Oral peptide drug delivery: polymer-inhibitor conjugates protecting insulin from enzymatic degradation in vitro. Biomaterials, 2000, 21(14), 1499-1507.
[http://dx.doi.org/10.1016/S0142-9612(00)00039-9] [PMID: 10872779] -4Yang, L.; Chu, J.S.; Fix, J.A. Colon-specific drug delivery: new approaches and in vitro/in vivo evaluation. Int. J. Pharm., 2002, 235(1-2), 1-15.
[http://dx.doi.org/10.1016/S0378-5173(02)00004-2] [PMID: 11879735] ]. Such effects can be avoided by using sublingual or buccal route [5Smart, JD Buccal drug delivery. Expert opinion on Drug Delivery. 2005, 2(3), 507-517.
[http://dx.doi.org/10.1517/17425247.2.3.507] ]. Buccal cavity presents a milder environment for drug, devoid of the acid hydrolysis and hepatic first pass effect [6Puratchikody, A; Mathew, ST. Buccal drug delivery: past, present and future-a review. Int. J. Drug Deliver, 2011, 3(4)] improved drug delivery and bioavailability [7Jain, A.C.; Aungst, B.J.; Adeyeye, M.C. Development and in vivo evaluation of buccal tablets prepared using danazol-sulfobutylether 7 β-cyclodextrin (SBE 7) complexes. J. Pharm. Sci., 2002, 91(7), 1659-1668.
[http://dx.doi.org/10.1002/jps.10163] [PMID: 12115827] ]. Moreover, it has been reported to improve drug delivery through buccal route and dosage form can be removed mechanically by hand in case of toxicity. The ideal polymeric combination provides both excellent release and better mucoadhesion with easy processing and lower cost [8Shojaei, A.H. Buccal mucosa as a route for systemic drug delivery: a review. J. Pharm. Pharm. Sci., 1998, 1(1), 15-30.
[PMID: 10942969] ].
Propranolol HCl, a non-selective therapeutic beta blocker and possesses beneficial effects in hypertension [9Sinagra, E.; Perricone, G.; DAmico, M.; Tinè, F.; DAmico, G. Systematic review with meta-analysis: the haemodynamic effects of carvedilol compared with propranolol for portal hypertension in cirrhosis. Aliment. Pharmacol. Ther., 2014, 39(6), 557-568.
[http://dx.doi.org/10.1111/apt.12634] [PMID: 24461301] ], angina [10Idrisova, E.M.; Boshchenko, A.A.; Borovkova, N.V.; Demochko, A.V.; Chernov, V.I.; Karpov, R.S. Propranolol treatment of effort angina in patients with arterial hypotension. Ter. Arkh., 2004, 76(8), 32-36.
[PMID: 15471393] ], cardiomyopathy, cardiac arrhythmia [11Puljević, M.; Velagić, V.; Puljević, D.; Miličić, D. Propranolol efficiency in prevention of sustained ventricular tachycardia in patients with implanted cardioverter-defibrillator: a case series. Croat. Med. J., 2014, 55(1), 75-76.
[http://dx.doi.org/10.3325/cmj.2014.55.75] [PMID: 24577831] ], anxiety [12Fourneret, P.; Desombre, H.; de Villard, R.; Revol, O. Interest of propranolol in the treatment of school refusal anxiety: about three clinical observations. Encephale, 2001, 27(6), 578-584.
[PMID: 11865565] ], hyperthyroidism [13Freitas, F.; Estato, V.; Lessa, M.A.; Tibiriçá, E. Cardiac microvascular rarefaction in hyperthyroid rats is reversed by losartan, diltiazem, and propranolol. Fundam. Clin. Pharmacol., 2015, 29(1), 31-40.
[PMID: 24689791] ], myocardial infarction [14Cunnington, C; McDonald, JE; Singh, RK Epinephrine-induced myocardial infarction in severe anaphylaxis: is nonselective β-blockade a contributory factor? Am. J. Emerg. Med., 2013, 31(4), 759-2.], migraine prophylaxis [15Millán-Guerrero, R.O.; Isais-Millán, R.; Guzmán-Chávez, B.; Castillo-Varela, G. N alpha methyl histamine versus propranolol in migraine prophylaxis. Can. J. Neurol. Sci., 2014, 41(2), 233-238.
[http://dx.doi.org/10.1017/S0317167100016632] [PMID: 24534036] ], anti-angiogenesis [16Xu, T.; Xiao, X.; Zheng, S.; Zheng, J.; Zhu, H.; Ji, Y.; Yang, S. Antiangiogenic effect of propranolol on the growth of the neuroblastoma xenografts in nude mice. J. Pediatr. Surg., 2013, 48(12), 2460-2465.
[http://dx.doi.org/10.1016/j.jpedsurg.2013.08.022] [PMID: 24314187] ] etc. The normal route of drug delivery is oral route. The drug has to undergo severe first pass metabolism effect as well as bioavailability range between 15 to 23% [17Cid, E.; Mella, F.; Lucchini, L.; Cárcamo, M.; Monasterio, J. Plasma concentrations and bioavailability of propranolol by oral, rectal, and intravenous administration in man. Biopharm. Drug Dispos., 1986, 7(6), 559-566.
[http://dx.doi.org/10.1002/bdd.2510070605] [PMID: 3828485] , 18Walle, T.; Conradi, E.C.; Walle, U.K.; Fagan, T.C.; Gaffney, T.E. The predictable relationship between plasma levels and dose during chronic propranolol therapy. Clin. Pharmacol. Ther., 1978, 24(6), 668-677.
[http://dx.doi.org/10.1002/cpt1978246668] [PMID: 710025] ] and relatively short half life i.e. 3-5 hours [21Patel, V.M.; Prajapati, B.G.; Patel, H.V.; Patel, K.M. Mucoadhesive bilayer tablets of propranolol hydrochloride. AAPS Pharm. Sci. Tech., 2007, 8(3), E77.
[http://dx.doi.org/10.1208/pt0803077] [PMID: 17915827] ]. It is untoward the therapy goals as a continuous effective concentration is mandatory at the receptor site. The drug is a suitable contender to be delivered through buccal route as buccal route offers relative availability into direct system absorption bypassing first pass effect.
The aim of the current research was to deliver a continuous release of propranolol HCl as mucoadhesive buccal tablet. For this, mucoadhesive buccal tablet was formulated using mucoadhesive polymers i.e. CMC, EC, HPMC and CP. All such polymers have been extensively studied and showed good mucoadhesion, swellability and effect on drug releasing properties in the present study [19Sudhakar, Y.; Kuotsu, K.; Bandyopadhyay, A.K. Buccal bioadhesive drug deliverya promising option for orally less efficient drugs. J. Control. Release, 2006, 114(1), 15-40.
[http://dx.doi.org/10.1016/j.jconrel.2006.04.012] [PMID: 16828915] , 20Salamat-Miller, N.; Chittchang, M.; Johnston, T.P. The use of mucoadhesive polymers in buccal drug delivery. Adv. Drug Deliv. Rev., 2005, 57(11), 1666-1691.
[http://dx.doi.org/10.1016/j.addr.2005.07.003] [PMID: 16183164] ]. The current work was carried out to formulate and evaluate the mucoadhesive buccal tablet in terms of physicochemical properties so as to release propranolol HCl in a continuous manner.
2. MATERIALS AND METHODS
2.1. Materials
Propranolol HCl was received as a gift from Munawar Pharmaceuticals Pvt. Limited Lahore (Pakistan). Carbopol® 934P, CMC high viscosity grade 500-2500 mPa and EC-100 were purchased from Glow Scientific Traders, Lahore.
2.2. Methods
The study was completed in three stages, preliminary, main study and confirmation study. The preliminary study was undertaken to select the method of preparation and an estimation of polymers for the delivery of the drug. In the main study, the selected factors were changed within some range of mucoadhesive ingredients in each formulation employing computer-aided approach, artificial neural network on different formula to find the optimized factors for quality attributes for propranolol buccal mucoadhesive tablet formulation. The dose of propranolol HCl was kept fixed throughout the study. The weight of the tablet was kept at 500 mg in each formulation except for preliminary study. All formulations in the study were punched by single punch automatic machine by applying a force of 2 tons for 20 seconds.
2.3. Preliminary Study
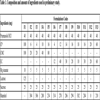
The formulation F1 was prepared using the wet granulation method while all others were punched by the direct compression method. The composition of propranolol HCl was 40 mg/tablet. The weight for each tablet designed in preliminary study was 400 mg as depicted in Table 1.
2.4. Evaluation Buccal Tablets in the Preliminary Study (F1-F14)
2.4.1. Physical Evaluation
About 400mg per tablet was compressed to a thickness of about 3 mm with a 12 mm diameter. Compressed tablets were tested for physical evaluation.
2.4.1.1. Surface pH
Surface pH of the tablet was examined by compact Inolab pH/ cond 720 (WTW). The tablets were kept in contact with distilled water for 2 h. and pH was observed by bringing the electrode in contact with the surface of tablet [22Bottenberg, P.; Cleymaet, R.; de Muynck, C.; Remon, J.P.; Coomans, D.; Michotte, Y.; Slop, D. Development and testing of bioadhesive, fluoride-containing slow-release tablets for oral use. J. Pharm. Pharmacol., 1991, 43(7), 457-464.
[http://dx.doi.org/10.1111/j.2042-7158.1991.tb03514.x] [PMID: 1682457] ]. The reading was taken when the pH of the system was stable. The procedure was repeated for different designated formulations.
2.4.1.2. Friability Test
Friability test on different formulations was performed using the Roche friabilitor according to USP [23Bhanja, S.; Ellaiah, P.; Martha, S.K.; Sahu, P.K.; Tiwari, S.P.; Panigrahi, B.B. Formulation and in vitro evaluation of mucoadhesive buccal tablets of Timolol maleate. Int. J. Pharm Biomed. Res., 2010, 1(4), 129-134.]. Results were expressed as the percentage loss as shown by Equation 1.
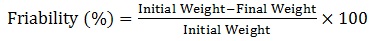 |
(1) |
2.4.1.3. Mucoadhesive Time
A set up similar to Syed et al. [24Hussain, A.; Syed, M.A.; Abbas, N.; Hanif, S.; Arshad, M.S.; Bukhari, N.I.; Hussain, K.; Akhlaq, M.; Ahmad, Z. Development of an ANN optimized mucoadhesive buccal tablet containing flurbiprofen and lidocaine for dental pain. Acta Pharm., 2016, 66(2), 245-256.
[http://dx.doi.org/10.1515/acph-2016-0020] [PMID: 27279067] ] was developed for the measurement of mucoadhesion time. For this purpose, pH of the testing solution was adjusted to pH 6.8 by Compact Inolab pH/ cond 720 (WTW). One face of the tablet was moistened with 50 μL phosphate buffer (pH 6.8) and forced gently against rabbit’s buccal mucosa which was stuck on the surface of the flat glass piece for 20 seconds. It was then positioned in a beaker containing 800 ml of buffer at 45o horizontally and stirred magnetically at 150 rpm (maintained at 37oC). The time of detachment of tablet was considered as in vitro mucoadhesive time [25Han, R-Y.; Fang, J-Y.; Sung, K.C.; Hu, O.Y. Mucoadhesive buccal disks for novel nalbuphine prodrug controlled delivery: effect of formulation variables on drug release and mucoadhesive performance. Int. J. Pharm., 1999, 177(2), 201-209.
[http://dx.doi.org/10.1016/S0378-5173(98)00343-3] [PMID: 10205614] ].
2.5. Main study (F14-F24)
Based on the preliminary study, composition of ingredients and method of tableting for the main study was decided. The composition of formulation, F3 (Table 1) was taken as formulation which could be manipulated further for the main study. The reason for the selection of F3 was its meetings of maximum specifications for a buccal dosage form. The formulations in preliminary study released the drug much earlier than the desired time due to which HPMC was added in the recipe. Since HPMC retards the release of the drug and has good mucoadhesion [26Karavas, E.; Georgarakis, E.; Bikiaris, D. Application of PVP/HPMC miscible blends with enhanced mucoadhesive properties for adjusting drug release in predictable pulsatile chronotherapeutics. Eur. J. Pharm. Biopharm., 2006, 64(1), 115-126.
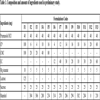
[http://dx.doi.org/10.1016/j.ejpb.2005.12.013] [PMID: 16675210] ]. It has been extensively used in the literature [26]. For that reason, it was added in the formulations in the main study (F14-F24). In the main study, the amounts of HPMC, CP, CMC, Na-alginate and EC had been changed to study its effect on formulation. A further aim of study was to find the optimized levels of the above factors to produce an optimized formulation. For this purpose, 11 different formulations (F14- F24) were prepared in the main study (Table 2).
2.6. Evaluation of Tablets in Main Study and Optimized Study
The formulations in the main study were evaluated with all the tests listed in the preliminary study. Additionally, in-vitro release, Swellability index and mucoadhesive strength were also performed on the formulations.
2.6.1. Mucoadhesive Strength
To quantify mucoadhesive strength of buccal tablet, a modified instrument was developed as shown in Fig. (1 ). One arm of the balance was replaced with thread with the help of which two glass slides were tide. The tablet was sandwiched between the slides as shown in Fig. (1
). One arm of the balance was replaced with thread with the help of which two glass slides were tide. The tablet was sandwiched between the slides as shown in Fig. (1 ). One glass slide was fixed while the other moveable glass slide the attached with arm of the balance to access the degree of mucoadhesion. Between glass slides, both surfaces of tablet were wetted with phosphate buffer solution (pH 6.8).
). One glass slide was fixed while the other moveable glass slide the attached with arm of the balance to access the degree of mucoadhesion. Between glass slides, both surfaces of tablet were wetted with phosphate buffer solution (pH 6.8).
 |
Fig. (1) Tablet mucoadhesive strength testing apparatus. |
On the left pan, drops of water were used in terms of weight to measure the force of detachment. When apparatus was in static equilibrium, water was added [27Mohammadi-Samani, S.; Bahri-Najafi, R.; Yousefi, G. Formulation and in vitro evaluation of prednisolone buccoadhesive tablets. Farmaco, 2005, 60(4), 339-344.
[http://dx.doi.org/10.1016/j.farmac.2005.01.009] [PMID: 15848210] ] until the slide detaches. The force was then accessed for mucoadhesion [28Gupta, A.; Gaud, R.S.; Ganga, S. Development, evaluation and optimization of extended release buccal tablets prepared using progressive hydration technology. Int. J. Drug Deliv., 2011, 2(1)]. Weight in grams was converted to Newton using Equation 2.
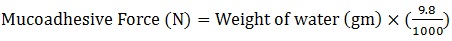 |
(2) |
2.6.2. Swellability Index
The water uptake by the mucoadhesive tablet was checked by calculating swellability index. Tablet was dipped in a Petri dish containing phosphate buffer (pH 6.8). The weight of the tablet was measured initially (W1) and then at every hour interval up to 6 h. The extent of increase in weight was related to water absorbed (W2) for each time. The percentage swellability was calculated by using Equation 3 [28Gupta, A.; Gaud, R.S.; Ganga, S. Development, evaluation and optimization of extended release buccal tablets prepared using progressive hydration technology. Int. J. Drug Deliv., 2011, 2(1)].
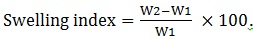 |
(3) |
2.6.3. In-vitro Drug Release
The in vitro release study was conducted in USP 28 Type 2 dissolution apparatus (ERWEKA DT-700) with a rotation of paddles at 50 rpm. 500 ml of phosphate buffer (pH 6.8) as dissolution medium was maintained at 37±0.5oC throughout the experiment. Samples were taken at 0.25, 0.5, 1, 2, 3, 4, 5 and 6 hour and measured against a calibration curve for the quantitative determination of propranolol HCl [29Edavalath, S; Rao, B Design, development and optimization of buccal bioadhesive tablets of diclofenac sodium for the treatment of odontalgia. Ars Pharm., 2011, 2011, 52(2), 05-13.].
2.7. Data Analysis by Artificial Neural Network (ANN)
Change in the quantity of polymers in formulations was considered as factors for varied response in properties such as hardness, weight variation, friability, diameter, thickness, surface pH, mucoadhesive time, mucoadhesive strength and in-vitro drug release through artificial intelligence using Neural power 3.1 [30Kurtaran, H.; Ozcelik, B.; Erzurumlu, T. Warpage optimization of a bus ceiling lamp base using neural network model and genetic algorithm. J. Mater Process. Tech., 2005, 169(2), 314-319.
[http://dx.doi.org/10.1016/j.jmatprotec.2005.03.013] ]. Desirability through optimization was generated using the approach “what if command” to predict concentration of polymers and a confirmation formulation was evaluated accordingly. For data analysis Incremental Back Propagation (IBP) method was used as learning algorithm. The connection type used for learning the trend in data was multilayer normal feed forward. The number of total layers and input layers were 3 and 6 respectively. The number of nodes in output layer were 10 using tanh as a non-linear transfer function.
The desirable values of different physicochemical parameters for the optimization of mucoadhesive tablet has been listed in Table 3. Note that the physiological pH of buccal cavity is around 6.5 so the desirability value would not damaging to the buccal mucosa. The tablet should be reasonably hard that it could release drug in a sustained manner. Similarly, the release of the drug was designed to be more than 65% till 6 hr.
2.8. Confirmation Study
The predicted levels (amounts) of factors, such as HPMC, EC, CMC, CP, Na-alginate and lactose generated by Neural Power 3.1 in the main study were tested experimentally by formulating the confirmation formulation based on prediction. Such formulation was tested for all the physicochemical tests as listed above.
2.9. Release Kinetics of Propranolol HCl
In vitro release kinetic model was studied on the release of propranolol HCl using software DD Solver®. The release data were fitted to zero order, 1st order Higuchi and Korsmeyer-Peppas release models. The best model was selected based on the highest R2 value [31Labib, G.S.; Farid, R.M. Osteogenic effect of locally applied Pentoxyfilline gel: in vitro and in vivo evaluations. Drug Deliv., 2014, (0), 1-9.
[PMID: 24555662] ] and results were interpreted. It was applied only to confirmation formulation.
3. RESULTS AND DISCUSSION
In preliminary study, CP and EC were used as mucoadhesive polymers and release retardant which has been used in different studies. The aim of the preliminary study was to find the appropriate method and an estimation of the appropriate ingredients of the buccal tablet of propranolol HCl. While formulating, F1 was prepared with wet granulation (Table 1) but it was dislodged immediately from the rabbit mucosa after its application in mucoadhesive time test. Thus wet granulation was not employed further rather all formulations including F1 were re-tableted by the direct compression method, the results of which have been expressed.
3.1. Physicochemical Characterization of Buccal Tablets in the Preliminary Study
A significant mucoadhesion time is required for the attachment of polymers to buccal mucosa so that drug can be released from matrix over time locally. For buccal tablet, the neutral pH is required to avoid irritation.
Results for hardness, thickness, diameter, surface, pH, mucoadhesive time and friability of the tablets prepared in the preliminary study are summarized in Table 4. Though F1 was prepared using wet as well as direct compression method, the results for F1 prepared by the direct compression method have been enlisted (Table 4). All the formulations from F1 to F13 demonstrated 4 to 7.5 kg/cm2 hardness, thickness 3 to 3.2 mm, diameter 12 to 12.3mm whereas friability was 0.5 to 0.7%. The mucoadhesive time ranges from 2 to 4 h. The average weight for all formulations in preliminary studies was ranged between 391.6 to 407.4 mg. The deviation of weight of the tablets was within the compendia limits according to USP 32. Surface pH in between 5.8 to 7.0 was considered to be in the physiological range of pH. The surface pH of all formulations was from 5 to7. Only formulations F1, F5, F6 were more acidic and outside the physiological pH range which might be due to the greater concentrations of CMC and CP used as shown in Table 4.
The required pH for propranolol HCl is 6.5 ± 0.05 [32Patel, V.M.; Prajapati, B.G.; Patel, M.M. Formulation, evaluation, and comparison of bilayered and multilayered mucoadhesive buccal devices of propranolol hydrochloride. AAPS Pharm. Sci. Tech., 2007, 8(1), 22.
[http://dx.doi.org/10.1208/pt0801022] [PMID: 17408221] ]. In the main study, HPMC was added so as to increase the mucoadhesion properties. Sucrose acted as a diluents, binder and sweetener, thus was kept in further formulation design in the main study
3.2. Physicochemical Characterization of Buccal Tablets in the Main Study
The aim of the main study was to find the levels of CP, EC, HPMC, SA and CMC for the production of an optimized buccal tablet of propranolol HCl. HPMC as a release retardant and mucoadhesive agent was additionally added in the study. Because the mucoadhesive time for tablet in the preliminary study was comparatively lower than the desired criteria due to which HPMC was predicted to increase mucoadhesion. It has been extensively used in buccal drug delivery and has proven satisfactory results [8Shojaei, A.H. Buccal mucosa as a route for systemic drug delivery: a review. J. Pharm. Pharm. Sci., 1998, 1(1), 15-30.
[PMID: 10942969] ]. The results from the main study are summarized in Table 5. As shown, the average weight and friability of all the formulations were within the USP limit of not more than 0.8%. The average weight of all formulations in the main study was also within in ±5% USP allowed deviation. The pH should be such that it should not disturb the local physiological functions because the buccal tablet has to reside a longer period of time. It should not convert the lining of mucosa into any pathological form being more acidic or so. As in Table 5, the pH of all formulations was within the physiological limit (5.8-7.0) except three [33M. S. Pendekal Ars Pharm P. K. Tegginamat. Formulation and evaluation of a bioadhesive patch for buccal delivery of tizanidine. Acta Pharm. Sin. B, 2012, 2, 318-324.
[http://dx.doi.org/10.1016/j.apsb.2011.12.012] ], F16, F18 and F19 which was 5.5 for all. The hardness of formulations was designed to be around 6-8 Kg/cm2 [34Choi, H-G.; Kim, C-K. Development of omeprazole buccal adhesive tablets with stability enhancement in human saliva. J. Control. Release, 2000, 68(3), 397-404.
[http://dx.doi.org/10.1016/S0168-3659(00)00276-5] [PMID: 10974393] ]. A greater value of hardness would alter the release and patterns of swelling of the tablets. The diameter and thickness of the tablets showed a deviation than 5%.
Time required by the tablet to detach from the oral mucosa is the mucoadhesive time [21Patel, V.M.; Prajapati, B.G.; Patel, H.V.; Patel, K.M. Mucoadhesive bilayer tablets of propranolol hydrochloride. AAPS Pharm. Sci. Tech., 2007, 8(3), E77.
[http://dx.doi.org/10.1208/pt0803077] [PMID: 17915827] ]. The mucoadhesive time of the tablet should be such that it should neither detach instantly from the mucosa due to slight pressure or may not as much strong in mucoadhesion that it may damage the mucosal layer due to sticking action. Highest mucoadhesive time was obtained with the formulations F19 (4.8 h) which was containing 10% of EC only. Higher time was also observed with formulation (F23) containing 5% each of CMC and EC; and 20% percent of HPMC.
In general, swelling behaviour for formulations F17, F18 and F19 was faster compared with the others. Formu-lations containing HPMC i.e. F22-F24 showed least expansion of the gel. Formulations containing low concentrations of CP exhibited greater fragmentation of the gel from the peripheries compared with formulations containing higher concentrations of CP [24Hussain, A.; Syed, M.A.; Abbas, N.; Hanif, S.; Arshad, M.S.; Bukhari, N.I.; Hussain, K.; Akhlaq, M.; Ahmad, Z. Development of an ANN optimized mucoadhesive buccal tablet containing flurbiprofen and lidocaine for dental pain. Acta Pharm., 2016, 66(2), 245-256.
[http://dx.doi.org/10.1515/acph-2016-0020] [PMID: 27279067] ].
The data obtained from the main Study was used as input to optimize ingredient’s output. For this purpose, NeuralPower® version 3.1, artificial neural network (ANN) software was used for prediction of the optimized levels of above polymers [35Takayama, K.; Morva, A.; Fujikawa, M.; Hattori, Y.; Obata, Y.; Nagai, T. Formula optimization of theophylline controlled-release tablet based on artificial neural networks. J. Control. Release, 2000, 68(2), 175-186.
[http://dx.doi.org/10.1016/S0168-3659(00)00248-0] [PMID: 10925126] ]. In this study, 11 tablet formulations, F14-F24 were prepared and buccal tablet formulation F25 was the confirmation formulation. The tests accomplished in addition to that performed in preliminary study included dissolution test, mucoadhesive strength. Results of different tests are summarized in Table 5. For in-vitro release, standard calibration curve was drawn for propranolol HCl in phosphate buffer (pH 6.8) at concentrations from 0.5 to 40 µg/ml and a regression value of 0.9998 was obtained at 289 nm.
3.3. Critical Factors Affecting the Physical Properties of Tablets
Relative importance generated by software of the factors affecting the overall properties of the buccal tablet formulations as shown in Fig. (2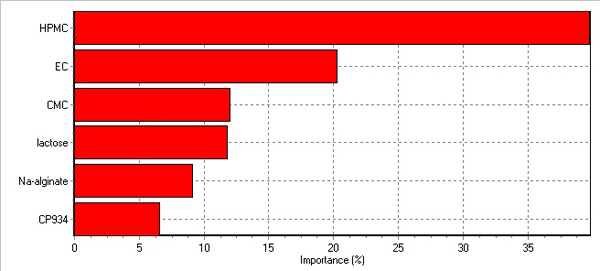 ). The two factors, viz, HPMC and EC exhibited more importance for the overall properties of the buccal tablet. The relative importance of CMC, lactose was equal to that of SA and CP showed little importance. Thus to achieve an optimized formulation, by manipulating the HPMC and EC, an optimized buccal table was achieved.
). The two factors, viz, HPMC and EC exhibited more importance for the overall properties of the buccal tablet. The relative importance of CMC, lactose was equal to that of SA and CP showed little importance. Thus to achieve an optimized formulation, by manipulating the HPMC and EC, an optimized buccal table was achieved.
 |
Fig. (2) Relative importance of HPMC, EC, CMC, lactose, Na-alginate and CP934 for different physicochemical properties of propranolol HCl generated by the optimization software, NeuralPower 3.1. |
The response surface plot of hardness test between HPMC and EC showed that changing amount of HPMC showed inverse relation with hardness of the tablet in the current study. The desired hardness can be achieved if lower amounts of HPMC is used along with higher concentrations of EC used in the study as depicted in Fig. (3a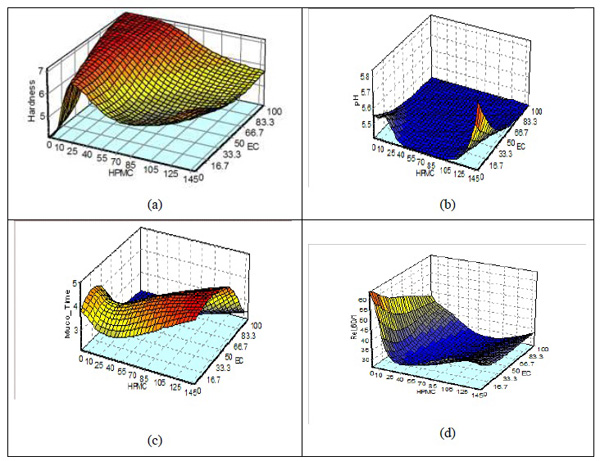 ).
).
The response surface plot showing the combined effect of HPMC and EC indicated the relative importance for physicochemical parameters. The surface pH of all buccal tablet formulations shown to be within the required pH, i.e., 5-7±0.2 [36S Pendekal M. K Tegginamat P. Formulation and evaluation of a bioadhesive patch for buccal delivery of tizanidine. Acta Pharm. Sin. B, 2012, 2(3), 318-324.
[http://dx.doi.org/10.1016/j.apsb.2011.12.012] ]. The response surface plot for surface pH showed that at higher level of HPMC and lower level of EC the pH was higher. The red region in Figs. (3b,c ) depicted that pH and mucoadhesive time were mainly dependant on the concentration of HPMC in the formulations. It meant that the increase in the concentration of HPMC was associated with increasing values of pH and mucoadhesion time. The blue colour corresponds to the area where least values of such tests were observed in the curve. The in vitro release was dependent upon the concentration of both polymers i.e. HPMC and EC where the release of drug was dependent upon the lowest concentration of the polymers. At higher concentration, little or least effect was evident at times 1 h 2 h and 3 h according to the surface plots as shown in Figs. (3d,e,f
) depicted that pH and mucoadhesive time were mainly dependant on the concentration of HPMC in the formulations. It meant that the increase in the concentration of HPMC was associated with increasing values of pH and mucoadhesion time. The blue colour corresponds to the area where least values of such tests were observed in the curve. The in vitro release was dependent upon the concentration of both polymers i.e. HPMC and EC where the release of drug was dependent upon the lowest concentration of the polymers. At higher concentration, little or least effect was evident at times 1 h 2 h and 3 h according to the surface plots as shown in Figs. (3d,e,f ). The release of drug at 4 h was mainly dependant on the concentration of EC where the increase in the concentration of polymer in the formulations was dependent upon the release of the drug as depicted in the red region in Fig. (3g
). The release of drug at 4 h was mainly dependant on the concentration of EC where the increase in the concentration of polymer in the formulations was dependent upon the release of the drug as depicted in the red region in Fig. (3g ). Conversely, the release of propranolol HCl at 5 h was dependent on the concentrations of both HPMC and EC. Where high impact of EC was found at 5 h and maximum release was relied on EC as shown in red region in Fig. (3h
). Conversely, the release of propranolol HCl at 5 h was dependent on the concentrations of both HPMC and EC. Where high impact of EC was found at 5 h and maximum release was relied on EC as shown in red region in Fig. (3h ).
).
3.4. Confirmation Formulation
The composition provided by the ANN was confirmed by formulating the predicted amounts of the ingredients. The predicted composition is provided in Table 6. The software also generated optimized values of the different physicochemical tests as provided in Table 7.
All the tests listed in method section were applied on the confirmation formulation. Additionally, swellability index and release kinetics were employed on the formulation. Results are summarized in Table 8. The formulation F25 showed hardness 8 kg/cm2, diameter 11.1 mm, thickness 3mm, surface pH 6.5, mucoadhesion time 3.9 h and release was 22% at 15 min, 26% at 30 min, 34% at1 h, 40% at 2 h, 45% at 3 h, 50% at 4 h, 62% at 5h, 76% at 6h, 85% at 7h and 97% at 8 h. However, a slight difference was noted in hardness, surface pH, mucoadhesive time and release profile compared with the predicted values generated by artificial intelligence.
A significant mucoadhesion is required or the attachment of tablet on to the mucosal membrane. Mucoadhesive strength of optimized formulation F25 was 0. 0338N which was comparable [21Patel, V.M.; Prajapati, B.G.; Patel, H.V.; Patel, K.M. Mucoadhesive bilayer tablets of propranolol hydrochloride. AAPS Pharm. Sci. Tech., 2007, 8(3), E77.
[http://dx.doi.org/10.1208/pt0803077] [PMID: 17915827] ]. Swellability index is the direct measurement of sorption of water into the mucoadhesive matrix. The ability of water intake by the polymers used in the formulations makes them swell and creates a passage for drugs to release either by erosion of the matrix or by movement of drug out of the intact matrix [37Boyapally, H.; Nukala, R.K.; Bhujbal, P.; Douroumis, D. Controlled release from directly compressible theophylline buccal tablets. Colloids Surf. B. Biointerfaces, 2010, 77(2), 227-233.
[http://dx.doi.org/10.1016/j.colsurfb.2010.01.031] [PMID: 20188529] ]. Swelling index continuously increased from 42% to more than 100% during time 1 h to 6 h reaching a plateau at 6 h. Swellable weight equal to the dry weight was achieved at 5 h. The maximum swelling was observed at 6 h as observed in Fig. (4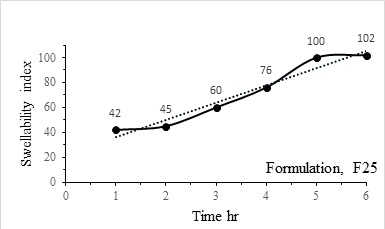 ).
).
 |
Fig. (4) Swellability index of Formulation, F25 with predicted trendline. |
3.5. In vitro Drug Release and Release Kinetics
The desirability of buccal tablet was to release the drug in a continuous manner upto 8 hours. This design was to avoid fluctuation of concentration of drug at the serum. Propranolol HCl is a potent drug and slighter change in the amounts of drug in plasma is associated with adverse effects [38Lardinois, C.K.; Neuman, S.L. The effects of antihypertensive agents on serum lipids and lipoproteins. Arch. Intern. Med., 1988, 148(6), 1280-1288.
[http://dx.doi.org/10.1001/archinte.1988.00380060044012] [PMID: 2897834] ]. So, a continuous release was preferred. The data was used for optimization of the ingredients. The release data for formulation F25 was taken up to 8 h based on the predicted release of at least 65.70% at 6 h, as given in Table 7. The in vitro release data is presented in Table 9. It revealed that the initial release was neither slow nor fast and at time 5 h, half of the drug was released from tablet matrix. The release of the drug was almost complete and at 8 h, more than 97% of propranolol HCl was released.
Kinetic behaviour of the confirmation formulation, F25 was studied using software “DD Solver. The coefficient of relationship (R2) values of the models are given in Table 10. Based on the highest R2 value, the Korsmeyer-Peppas model (Fig. 5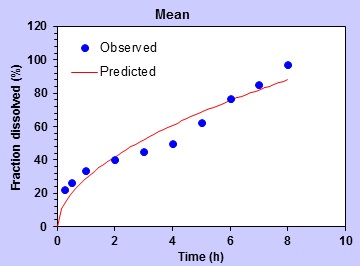 ) fitted the release data well and has been indicated in Fig. (4
) fitted the release data well and has been indicated in Fig. (4 ). The n value of the formulation F25 was found to be 0.534 (R2 = 0.9235) which suggests the non-Fickian drug release [39Pygall, S.R.; Kujawinski, S.; Timmins, P.; Melia, C.D. Mechanisms of drug release in citrate buffered HPMC matrices. Int. J. Pharm., 2009, 370(1-2), 110-120.
). The n value of the formulation F25 was found to be 0.534 (R2 = 0.9235) which suggests the non-Fickian drug release [39Pygall, S.R.; Kujawinski, S.; Timmins, P.; Melia, C.D. Mechanisms of drug release in citrate buffered HPMC matrices. Int. J. Pharm., 2009, 370(1-2), 110-120.
[http://dx.doi.org/10.1016/j.ijpharm.2008.11.022] [PMID: 19100822] ]. Such a system shows that the rate of drug diffusion and the polymer erosion are same [40Dash, S.; Murthy, P.N.; Nath, L.; Chowdhury, P. Kinetic modeling on drug release from controlled drug delivery systems. Acta Pol. Pharm., 2010, 67(3), 217-223.
[PMID: 20524422] ]. It suggests that drug is released by an “initial burst” and drug resides in the surrounding gel layer of the polymer. After that erosion of polymer will take place following the diffusion of drug into the dissolution medium [39Pygall, S.R.; Kujawinski, S.; Timmins, P.; Melia, C.D. Mechanisms of drug release in citrate buffered HPMC matrices. Int. J. Pharm., 2009, 370(1-2), 110-120.
[http://dx.doi.org/10.1016/j.ijpharm.2008.11.022] [PMID: 19100822] ]. The amount of the drug released depends upon the penetration of dissolution medium through the surrounding gel of CP into the HPMC matrix.
 |
Fig. (5) Fitting of release of propranolol HCl in optimized formulation, F25 according to Korsmeyer-Peppas Model. |
CONCLUSION
The buccal anti-hypertensive tablet of propranolol HCl was prepared by the direct compression using mucoadhesive polymeric combination of CP, EC, CMC and HPMC. It was concluded that drug release observed to be faster with the increase in concentration of HPMC. The swellability was controlled BY CP gel surrounding the HPMC matrix. The formulation was optimized for maximum release and physicochemical characters for desired period of time using NeuralPower 3.1. Results revealed that HPMC imparted greater importance on physicochemical parameters like in vitro drug release, swellability and mucoadhesion compared with the other. It can be concluded that buccal mucoadhesive tablet for the continuous release of propranolol HCl can be an effective option to deliver the drug through mucoadhesive buccal route.
CONFLICT OF INTEREST
The authors confirm that this article content has no conflict of interest.
ACKNOWLEDGEMENTS
Declared none.
REFERENCES
| [1] | Varadarajulu, S.; Tamhane, A.; Drelichman, E.R. Patient perception of natural orifice transluminal endoscopic surgery as a technique for cholecystectomy. Gastrointest. Endosc., 2008, 67(6), 854-860. [http://dx.doi.org/10.1016/j.gie.2007.09.053] [PMID: 18355816] |
| [2] | Marschütz, M.K.; Bernkop-Schnürch, A. Oral peptide drug delivery: polymer-inhibitor conjugates protecting insulin from enzymatic degradation in vitro. Biomaterials, 2000, 21(14), 1499-1507. [http://dx.doi.org/10.1016/S0142-9612(00)00039-9] [PMID: 10872779] |
| [3] | Maroni, A.; Del Curto, M.D.; Zema, L.; Foppoli, A.; Gazzaniga, A. Film coatings for oral colon delivery. Int. J. Pharm., 2013, 457(2), 372-394. [http://dx.doi.org/10.1016/j.ijpharm.2013.05.043] [PMID: 23727142] |
| [4] | Yang, L.; Chu, J.S.; Fix, J.A. Colon-specific drug delivery: new approaches and in vitro/in vivo evaluation. Int. J. Pharm., 2002, 235(1-2), 1-15. [http://dx.doi.org/10.1016/S0378-5173(02)00004-2] [PMID: 11879735] |
| [5] | Smart, JD Buccal drug delivery. Expert opinion on Drug Delivery. 2005, 2(3), 507-517. [http://dx.doi.org/10.1517/17425247.2.3.507] |
| [6] | Puratchikody, A; Mathew, ST. Buccal drug delivery: past, present and future-a review. Int. J. Drug Deliver, 2011, 3(4) |
| [7] | Jain, A.C.; Aungst, B.J.; Adeyeye, M.C. Development and in vivo evaluation of buccal tablets prepared using danazol-sulfobutylether 7 β-cyclodextrin (SBE 7) complexes. J. Pharm. Sci., 2002, 91(7), 1659-1668. [http://dx.doi.org/10.1002/jps.10163] [PMID: 12115827] |
| [8] | Shojaei, A.H. Buccal mucosa as a route for systemic drug delivery: a review. J. Pharm. Pharm. Sci., 1998, 1(1), 15-30. [PMID: 10942969] |
| [9] | Sinagra, E.; Perricone, G.; DAmico, M.; Tinè, F.; DAmico, G. Systematic review with meta-analysis: the haemodynamic effects of carvedilol compared with propranolol for portal hypertension in cirrhosis. Aliment. Pharmacol. Ther., 2014, 39(6), 557-568. [http://dx.doi.org/10.1111/apt.12634] [PMID: 24461301] |
| [10] | Idrisova, E.M.; Boshchenko, A.A.; Borovkova, N.V.; Demochko, A.V.; Chernov, V.I.; Karpov, R.S. Propranolol treatment of effort angina in patients with arterial hypotension. Ter. Arkh., 2004, 76(8), 32-36. [PMID: 15471393] |
| [11] | Puljević, M.; Velagić, V.; Puljević, D.; Miličić, D. Propranolol efficiency in prevention of sustained ventricular tachycardia in patients with implanted cardioverter-defibrillator: a case series. Croat. Med. J., 2014, 55(1), 75-76. [http://dx.doi.org/10.3325/cmj.2014.55.75] [PMID: 24577831] |
| [12] | Fourneret, P.; Desombre, H.; de Villard, R.; Revol, O. Interest of propranolol in the treatment of school refusal anxiety: about three clinical observations. Encephale, 2001, 27(6), 578-584. [PMID: 11865565] |
| [13] | Freitas, F.; Estato, V.; Lessa, M.A.; Tibiriçá, E. Cardiac microvascular rarefaction in hyperthyroid rats is reversed by losartan, diltiazem, and propranolol. Fundam. Clin. Pharmacol., 2015, 29(1), 31-40. [PMID: 24689791] |
| [14] | Cunnington, C; McDonald, JE; Singh, RK Epinephrine-induced myocardial infarction in severe anaphylaxis: is nonselective β-blockade a contributory factor? Am. J. Emerg. Med., 2013, 31(4), 759-2. |
| [15] | Millán-Guerrero, R.O.; Isais-Millán, R.; Guzmán-Chávez, B.; Castillo-Varela, G. N alpha methyl histamine versus propranolol in migraine prophylaxis. Can. J. Neurol. Sci., 2014, 41(2), 233-238. [http://dx.doi.org/10.1017/S0317167100016632] [PMID: 24534036] |
| [16] | Xu, T.; Xiao, X.; Zheng, S.; Zheng, J.; Zhu, H.; Ji, Y.; Yang, S. Antiangiogenic effect of propranolol on the growth of the neuroblastoma xenografts in nude mice. J. Pediatr. Surg., 2013, 48(12), 2460-2465. [http://dx.doi.org/10.1016/j.jpedsurg.2013.08.022] [PMID: 24314187] |
| [17] | Cid, E.; Mella, F.; Lucchini, L.; Cárcamo, M.; Monasterio, J. Plasma concentrations and bioavailability of propranolol by oral, rectal, and intravenous administration in man. Biopharm. Drug Dispos., 1986, 7(6), 559-566. [http://dx.doi.org/10.1002/bdd.2510070605] [PMID: 3828485] |
| [18] | Walle, T.; Conradi, E.C.; Walle, U.K.; Fagan, T.C.; Gaffney, T.E. The predictable relationship between plasma levels and dose during chronic propranolol therapy. Clin. Pharmacol. Ther., 1978, 24(6), 668-677. [http://dx.doi.org/10.1002/cpt1978246668] [PMID: 710025] |
| [19] | Sudhakar, Y.; Kuotsu, K.; Bandyopadhyay, A.K. Buccal bioadhesive drug deliverya promising option for orally less efficient drugs. J. Control. Release, 2006, 114(1), 15-40. [http://dx.doi.org/10.1016/j.jconrel.2006.04.012] [PMID: 16828915] |
| [20] | Salamat-Miller, N.; Chittchang, M.; Johnston, T.P. The use of mucoadhesive polymers in buccal drug delivery. Adv. Drug Deliv. Rev., 2005, 57(11), 1666-1691. [http://dx.doi.org/10.1016/j.addr.2005.07.003] [PMID: 16183164] |
| [21] | Patel, V.M.; Prajapati, B.G.; Patel, H.V.; Patel, K.M. Mucoadhesive bilayer tablets of propranolol hydrochloride. AAPS Pharm. Sci. Tech., 2007, 8(3), E77. [http://dx.doi.org/10.1208/pt0803077] [PMID: 17915827] |
| [22] | Bottenberg, P.; Cleymaet, R.; de Muynck, C.; Remon, J.P.; Coomans, D.; Michotte, Y.; Slop, D. Development and testing of bioadhesive, fluoride-containing slow-release tablets for oral use. J. Pharm. Pharmacol., 1991, 43(7), 457-464. [http://dx.doi.org/10.1111/j.2042-7158.1991.tb03514.x] [PMID: 1682457] |
| [23] | Bhanja, S.; Ellaiah, P.; Martha, S.K.; Sahu, P.K.; Tiwari, S.P.; Panigrahi, B.B. Formulation and in vitro evaluation of mucoadhesive buccal tablets of Timolol maleate. Int. J. Pharm Biomed. Res., 2010, 1(4), 129-134. |
| [24] | Hussain, A.; Syed, M.A.; Abbas, N.; Hanif, S.; Arshad, M.S.; Bukhari, N.I.; Hussain, K.; Akhlaq, M.; Ahmad, Z. Development of an ANN optimized mucoadhesive buccal tablet containing flurbiprofen and lidocaine for dental pain. Acta Pharm., 2016, 66(2), 245-256. [http://dx.doi.org/10.1515/acph-2016-0020] [PMID: 27279067] |
| [25] | Han, R-Y.; Fang, J-Y.; Sung, K.C.; Hu, O.Y. Mucoadhesive buccal disks for novel nalbuphine prodrug controlled delivery: effect of formulation variables on drug release and mucoadhesive performance. Int. J. Pharm., 1999, 177(2), 201-209. [http://dx.doi.org/10.1016/S0378-5173(98)00343-3] [PMID: 10205614] |
| [26] | Karavas, E.; Georgarakis, E.; Bikiaris, D. Application of PVP/HPMC miscible blends with enhanced mucoadhesive properties for adjusting drug release in predictable pulsatile chronotherapeutics. Eur. J. Pharm. Biopharm., 2006, 64(1), 115-126. [http://dx.doi.org/10.1016/j.ejpb.2005.12.013] [PMID: 16675210] |
| [27] | Mohammadi-Samani, S.; Bahri-Najafi, R.; Yousefi, G. Formulation and in vitro evaluation of prednisolone buccoadhesive tablets. Farmaco, 2005, 60(4), 339-344. [http://dx.doi.org/10.1016/j.farmac.2005.01.009] [PMID: 15848210] |
| [28] | Gupta, A.; Gaud, R.S.; Ganga, S. Development, evaluation and optimization of extended release buccal tablets prepared using progressive hydration technology. Int. J. Drug Deliv., 2011, 2(1) |
| [29] | Edavalath, S; Rao, B Design, development and optimization of buccal bioadhesive tablets of diclofenac sodium for the treatment of odontalgia. Ars Pharm., 2011, 2011, 52(2), 05-13. |
| [30] | Kurtaran, H.; Ozcelik, B.; Erzurumlu, T. Warpage optimization of a bus ceiling lamp base using neural network model and genetic algorithm. J. Mater Process. Tech., 2005, 169(2), 314-319. [http://dx.doi.org/10.1016/j.jmatprotec.2005.03.013] |
| [31] | Labib, G.S.; Farid, R.M. Osteogenic effect of locally applied Pentoxyfilline gel: in vitro and in vivo evaluations. Drug Deliv., 2014, (0), 1-9. [PMID: 24555662] |
| [32] | Patel, V.M.; Prajapati, B.G.; Patel, M.M. Formulation, evaluation, and comparison of bilayered and multilayered mucoadhesive buccal devices of propranolol hydrochloride. AAPS Pharm. Sci. Tech., 2007, 8(1), 22. [http://dx.doi.org/10.1208/pt0801022] [PMID: 17408221] |
| [33] | M. S. Pendekal Ars Pharm P. K. Tegginamat. Formulation and evaluation of a bioadhesive patch for buccal delivery of tizanidine. Acta Pharm. Sin. B, 2012, 2, 318-324. [http://dx.doi.org/10.1016/j.apsb.2011.12.012] |
| [34] | Choi, H-G.; Kim, C-K. Development of omeprazole buccal adhesive tablets with stability enhancement in human saliva. J. Control. Release, 2000, 68(3), 397-404. [http://dx.doi.org/10.1016/S0168-3659(00)00276-5] [PMID: 10974393] |
| [35] | Takayama, K.; Morva, A.; Fujikawa, M.; Hattori, Y.; Obata, Y.; Nagai, T. Formula optimization of theophylline controlled-release tablet based on artificial neural networks. J. Control. Release, 2000, 68(2), 175-186. [http://dx.doi.org/10.1016/S0168-3659(00)00248-0] [PMID: 10925126] |
| [36] | S Pendekal M. K Tegginamat P. Formulation and evaluation of a bioadhesive patch for buccal delivery of tizanidine. Acta Pharm. Sin. B, 2012, 2(3), 318-324. [http://dx.doi.org/10.1016/j.apsb.2011.12.012] |
| [37] | Boyapally, H.; Nukala, R.K.; Bhujbal, P.; Douroumis, D. Controlled release from directly compressible theophylline buccal tablets. Colloids Surf. B. Biointerfaces, 2010, 77(2), 227-233. [http://dx.doi.org/10.1016/j.colsurfb.2010.01.031] [PMID: 20188529] |
| [38] | Lardinois, C.K.; Neuman, S.L. The effects of antihypertensive agents on serum lipids and lipoproteins. Arch. Intern. Med., 1988, 148(6), 1280-1288. [http://dx.doi.org/10.1001/archinte.1988.00380060044012] [PMID: 2897834] |
| [39] | Pygall, S.R.; Kujawinski, S.; Timmins, P.; Melia, C.D. Mechanisms of drug release in citrate buffered HPMC matrices. Int. J. Pharm., 2009, 370(1-2), 110-120. [http://dx.doi.org/10.1016/j.ijpharm.2008.11.022] [PMID: 19100822] |
| [40] | Dash, S.; Murthy, P.N.; Nath, L.; Chowdhury, P. Kinetic modeling on drug release from controlled drug delivery systems. Acta Pol. Pharm., 2010, 67(3), 217-223. [PMID: 20524422] |